L. Dowling1, E. McCloskey1, D.J. Cuthbertson2, J.S. Walsh1
1. The University of Sheffield, Sheffield, UK; 2. The University of Liverpool, Liverpool, UK.
Corresponding Author: Lisa Dowling, University of Sheffield Medical School, Beech Hill Road, S10 2RX, UK, lmdowling1@sheffield.ac.uk
J Frailty Aging 2023;12(1)37-42
Published online March 1, 2022, http://dx.doi.org/10.14283/jfa.2022.18
Abstract
Background: Obesity and low muscle strength (dynapenia) are independently associated with greater falls risk. It remains unclear whether dynapenia and obesity have an additive effect on falls risk, greater than either phenotype alone. Objectives: To determine whether a combination of abdominal obesity with dynapenia, dynapenic abdominal obesity (DAO), confers a greater risk of falls than either obesity or dynapenia alone in both men and women.
Design: An observational cohort study was conducted. Setting and Participants: Data from English adults (n=4239, 60-87 years) who took part in the English Longitudinal Study of Ageing were included. Measurements: Dynapenia, was defined as hand-grip strength <20kg (female), <30kg (male). Abdominal obesity was defined as waist circumference >88cm (female), >102cm (male). Data on falls and fall-related injuries over a 2-year follow-up were collected. Multiple logistic regression analyses were performed adjusting for age and sex, with results expressed as odds ratios (OR) and areas under the receiver operating characteristic curve (AUC).
Results: Falls occurred in 1049 participants, with 284 reporting a related injury during follow-up. DAO was associated with greater OR of falls in men (OR 2.1, 95% Confidence Intervals (CI) 1.3–3.2). Dynapenia rather than obesity was associated with falls in women, with greatest OR observed in those with low hand-grip strength (OR 1.4, 95% CI 1.1–1.7). Individual discrimination was low for measures of obesity or dynapenia either alone or in combination (AUC 0.51–0.58). There was no relationship between fall-related injuries and obesity or dynapenia.
Conclusion: Our findings suggest a synergistic effect of obesity with dynapenia on falls risk in men but not women.
Key words: Dynapenia, obesity, falls, ageing.
Introduction
Falls are a major public health concern for older adults. Approximately 30% of older adults (> 65 years) fall yearly (1). Worldwide data suggest that five percent of falls result in fracture and 30-50% of falls may result in minor injury (2). Falls and their consequences represent a huge economic burden to the UK National Health Service, estimated at £2.3bn yearly (1). With an ageing population, there is a growing need to be able to identify people predisposed to falls (fallers) in order to implement fall prevention strategies.
Individually, abdominal obesity (3, 4) and dynapenia (poor muscle strength) (5, 6) are associated with a greater risk of falling. Dynapenic abdominal obesity (DAO) is a phenotype of both low muscle strength and abdominal adiposity (7-9) thought to have the cumulative risk of both dynapenia and obesity. DAO is associated with worsening disability (7), hospitalisation (8), and mortality risk (9) and some studies suggest that individuals with DAO have a greater risk of falling than those with either obesity or dynapenia alone (10-12). However, these studies on falls were small and did not consider if there were differences between men and women.
DAO may be a more clinically relevant phenotype given the already well-established adverse effects of central adiposity (13). Moreover, excess body fat, particularly abdominally, can exacerbate both dynapenia (14, 15) and frailty (16). This may relate to the low grade inflammation associated with obesity which can exacerbate loss of muscle mass and promote fat mass gain (15, 17).
Whether there is a cumulative risk of both dynapenia and obesity on falls risk requires further consideration. In this study, our primary aim was to determine whether DAO conferred a greater risk of falls than either obesity or dynapenia alone in both men and women. We hypothesised that men and women with both dynapenic and obese phenotypes have a greater risk of falling.
Methods
Participants
A description of the English Longitudinal Study of Ageing (ELSA) has previously been published (18). In response to an ageing population, ELSA was designed to provide high quality longitudinal data in research areas focused on social status, physical and mental health, cognitive function and biology, in order to inform policy (18). Briefly, participants living in England were drawn by postcode and stratified by health authority and socioeconomic status. The survey began in 2002/3 with subsequent waves at two-yearly intervals. Refreshment samples were added to maintain representativeness of people aged 50-75 years. ELSA is the first longitudinal study of older adults in England which is broadly representative of the English population (18).
Data collection
Data collected by ELSA includes information on health, disability, economic status, social support and household structure (18). The main survey encompassed a face-to-face interview and paper self-completion questionnaire. Subsequent follow up occurred at different time points in ‘waves’. At waves 2, 4, 6 and 8, eligible participants (those who remained living in private households in England) were offered a follow-up visit by a qualified nurse. All participants gave written informed consent. For this present analysis we used the anthropometric measures, functional tests, sociodemographic and clinical characteristics at wave 6 (2012/13) as our baseline and self-reported falls at wave 7 (2014/15) as our outcome measure i.e. after a 2 year follow up period. These waves had the most complete data for the relationships we wanted to study. Exclusion criteria were applied to the potential participants as described in Fig. 1.
Measures
Falls and injuries
At wave 7 participants aged 60 years and above were asked if, for any reason, they had fallen in the past two years or since the date of their last interview. This question was used to derive an outcome variable for incident falls since baseline (wave 6). If participants responded that they had fallen in the past two years, they were subsequently asked whether that fall resulted in an injury that required medical attention. Participants who could not recall whether they had a fall or injury were assumed to not have had a fall or injury in the analysis.
Independent variables
Sociodemographic factors included age and sex. Available self-reported data on co-morbidities included “diabetes or high blood sugar”, coronary heart disease (CHD), arthritis (including osteoarthritis and rheumatism) and stroke (cerebrovascular disease). BMI was calculated as weight (kg) divided by height (m2). Two measurements of waist circumference (WC) were recorded; a third was taken if the initial two measurements differed by 3cm or more. The average of these measurements was used in the analyses. Three measurements of grip strength were taken on both dominant and non-dominant hands using an isometric hand-grip strength device (Smedley) and a standing position was used for the majority of participants (19). The maximum of these measurements was recorded as maximum hand-grip strength (HGS). A minimum of three hand-grip strength measurements was required for inclusion in this present study. The time taken to stand up and sit down five times from a firm chair without using arms was recorded as sit-to-stand (STS) time.
Dynapenia, obesity and dynapenic obesity
Dynapenia was defined as a hand-grip strength <20kg for women and <30kg for men (20), abdominal obesity as waist circumference >88cm for women and >102cm for men (21) and dynapenic abdominal obesity as the presence of both dynapenia and abdominal obesity. All participants were classed into one of four sub-groups (normal weight/non-dynapenic, dynapenic only, abdominal obese only and dynapenic abdominal obese).
EWGSOP2 criteria for dynapenia
Exploratory analysis was undertaken to determine whether alternative EWGSOP2 consensus measures of dynapenia (STS <15s; hand-grip strength <16kg for women and <27kg for men) (22) were also predictive of falls.
Statistical Analysis
Comparison between two groups was undertaken using either an independent t-test or Mann-Whitney U test; a chi-square test was used for categorical variables. Comparison between more than two groups was conducted using either one-way analysis of variance (ANOVA) with Tukey’s post hoc test or Kruskal-Wallis test with Dunn’s post hoc test. Multiple logistic regression was used to examine the association between measures of obesity, dynapenia or dynapenic abdominal obesity and incident falls in the next two years. Regression models were adjusted for age and sex, with results expressed as odds-ratios (OR) and discriminatory ability expressed as the area under the receiver operating characteristic curve (AUC). Significance was accepted at p<0.05. Analysis was undertaken using Stata V16.1 (StataCorp 2019).
To address our aims, the following models were used
Individual variable models
Measures of obesity and dynapenia were explored separately as continuous or categorical variables. For continuous measures of dynapenia or obesity, Z-scores were calculated as an individual’s result minus the population mean, divided by the population standard deviation. The use of Z-scores aimed to allow greater comparability between measures with different units e.g. centimetres, kilograms. Categorical variables of obesity and dynapenia were dichotomous for presence or absence of the phenotype according to consensus definitions. The non-obese or non-dynapenic groups were used as the reference group for the relevant analyses.
DAO models
The four sub-groups previously described, namely non-obese/non-dynapenic, dynapenic only, abdominal obese only, and DAO were included. The non-obese/non-dynapenic groups were used as the reference groups.
Results
Baseline characteristics
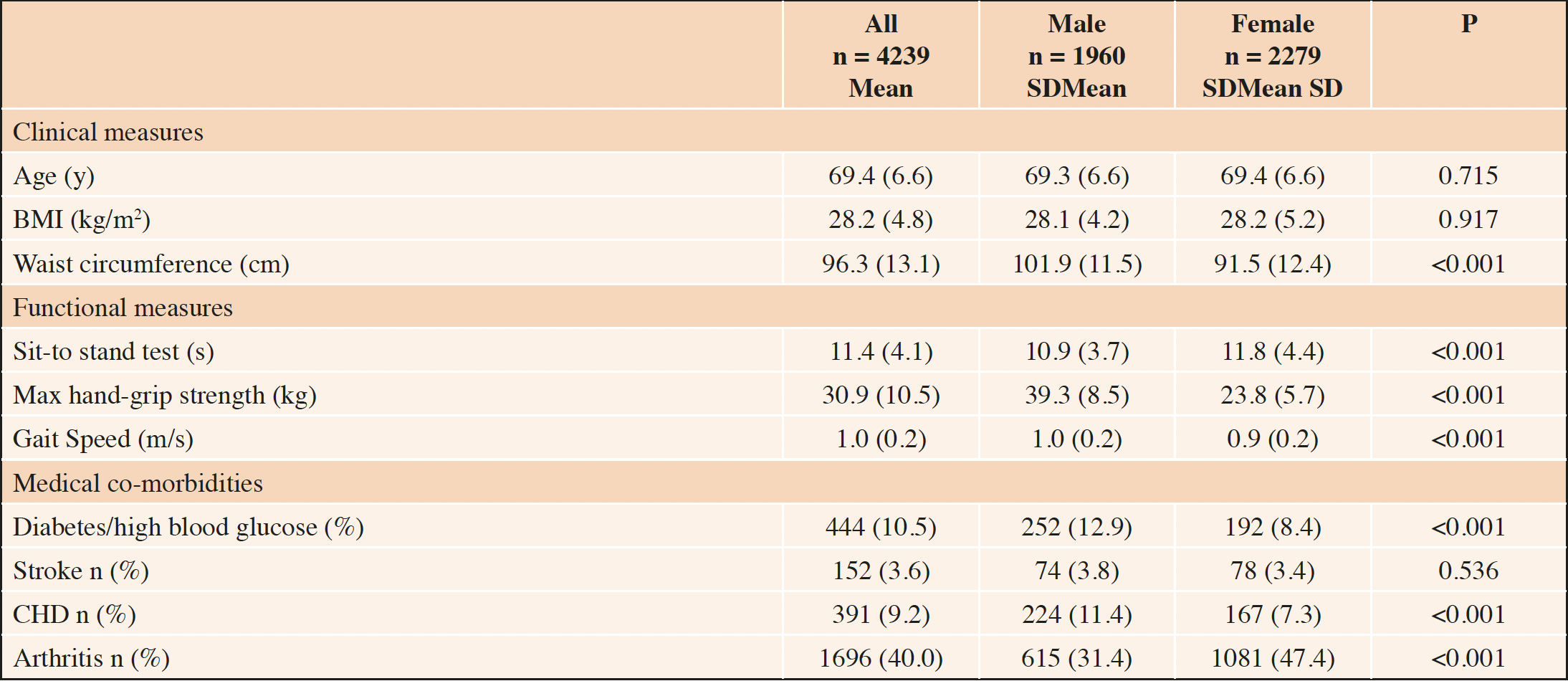
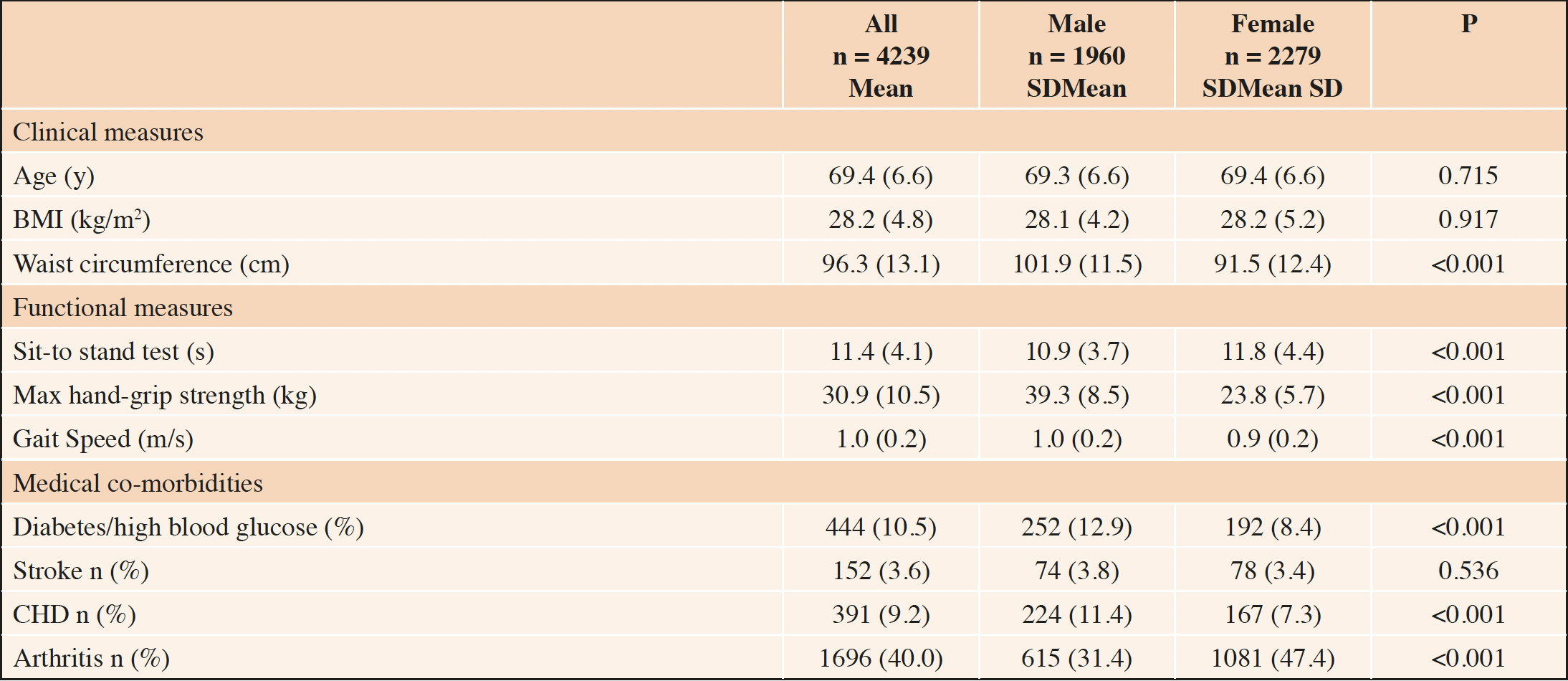
A total of 8054 participants took part in the interviews and nurse visits at wave 6. Of the 5911 adults aged ≥60 years, 4239 adults aged 60-87 years had the complete data necessary for the analysis at waves 6 and 7 (Fig. 1). Of these, 46% were male and 54% female (Table 1). Body mass index was similar between male and female participants, however men had greater waist circumference, hand-grip strength and quicker sit-to-stand times. More male participants reported that they had “diabetes or high blood sugar” or coronary heart disease (12.9% and 11.4%, respectively) than women (8.4% and 7.3%, respectively). More women reported that they had arthritis (including osteoarthritis and rheumatism; 47.4%) than men (31.4%). A similar proportion of men and women reported previously having a stroke (cerebral vascular disease).
* Participants were excluded if they were < 60 years old (n=2143), had either no measurement, an incomplete or a zero measurement for waist circumference (n=0), body mass index or body mass index < 18.5kg/m2 (n = 241), hand-grip strength (n=112), sit-to-stand time (n=789) or if they had refused to answer the question about falls in the previous 2 years (n=0). ** 530 participants were excluded if they did not complete, or refused to answer, the question about falls in the previous 2 years.
Characteristics are presented as mean and standard deviation or n (%). P-value refers to comparisons between men and women. Abbreviations: BMI = Body Mass Index; CHD = Coronary Heart Disease (angina or myocardial infarction). Note: 4035 participants had gait speed measurements.
Prevalence of abdominal obesity and dynapenia
According to waist circumference, 53% (n=2241) were obese (59% of women, 46% of men, p<0.001). The proportion of adults with dynapenia was 16.9% (n=720; 21% of women, 13% of men, p<0.001).
Incident falls
Twenty five percent of participants (n=1049) reported one or more falls in the two years between waves 6 and 7. Of those who fell, 60.5% fell once and 21.4% fell twice. More women fell (n=636, 28%) than men (n=413, 21%; p<0.001) but men reported a higher average number of falls (3.1 ± 11.7) than women (2.1 ± 8.2; p=0.047). Of those who fell, 27% (n=284) reported an injury that required medical attention; more women who fell reported injury (n=197, 31%) than men (n=87, 21%, p<0.001).
Association between falls, dynapenia and obesity
The associations between abdominal obesity and dynapenia as continuous variables, and falls incidence, are shown in Table 2. In the whole cohort, abdominal obesity and dynapenia were individually associated with falls incidence. A clear difference in the associations emerged when the analyses were explored by sex. Higher waist circumference was significantly predictive of falls in men but not women. Lower hand-grip strength showed similar relationships with falls incidence in men and women but, in contrast to the overall analysis, did not reach statistical significance in either sex.
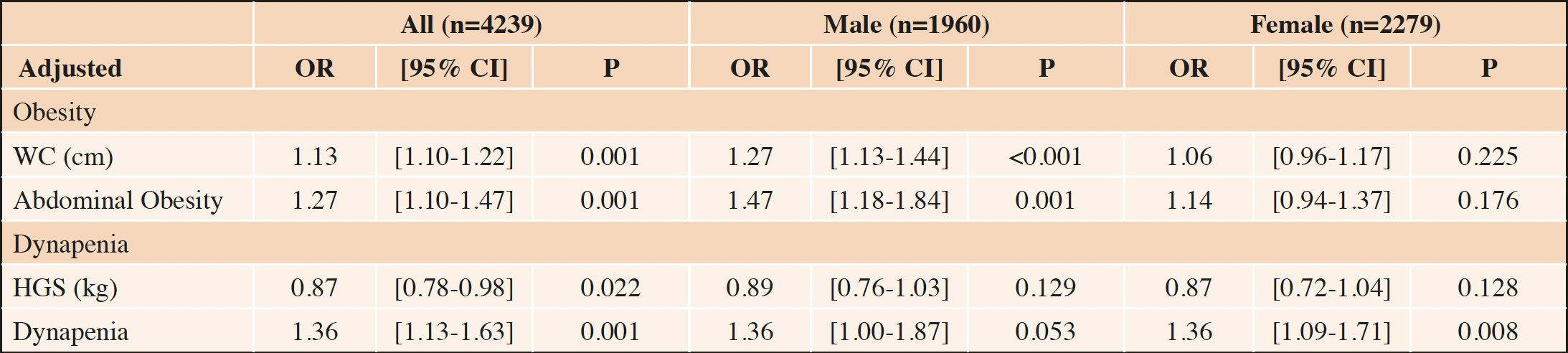
Table 2. Associations (expressed as odds ratios) between continuous measures (Z-scores) and consensus definitions of abdominal obesity or dynapenia and falls, by sex
Logistic regression models adjusted for age and sex. Abdominal obesity is defined as WC >88cm for women, >102cm for men; comparison is made to the reference non-abdominal obese group. Dynapenia is defined as HGS <20kg for women, <30kg for men; comparison is made to the reference non-dynapenic group. Abbreviations: OR = odds ratio; CI = confidence interval; WC = Waist Circumference; HGS = Hand-grip strength.
Next, we categorised participants according to the consensus definitions of abdominal obesity and dynapenia and examined the association with falls (Table 2). Similar patterns emerged whereby abdominal obesity was associated with falls in men but not women. Low HGS predicted falls in women but not in men.
Association between falls and dynapenic abdominal obesity
According to the definition of DAO, participants were normal weight (neither obese nor dynapenic) (n=1671, 45.2% female), dynapenic only (n=327, 57.8% female), abdominal obese only (n=1848, 56.9% female), and DAO (n=393, 72.3% female). Waist circumference and BMI were similar between normal weight or obese groups with and without dynapenia. However, men who were classified as having DAO had a lower BMI (29.8 ± 3.1 kg/m2) than the obese only group (31.4 ± 3.9 kg/m2; p=0.0098). Dynapenic and DAO sub-groups were significantly older than normal weight and obese sub-groups, respectively.
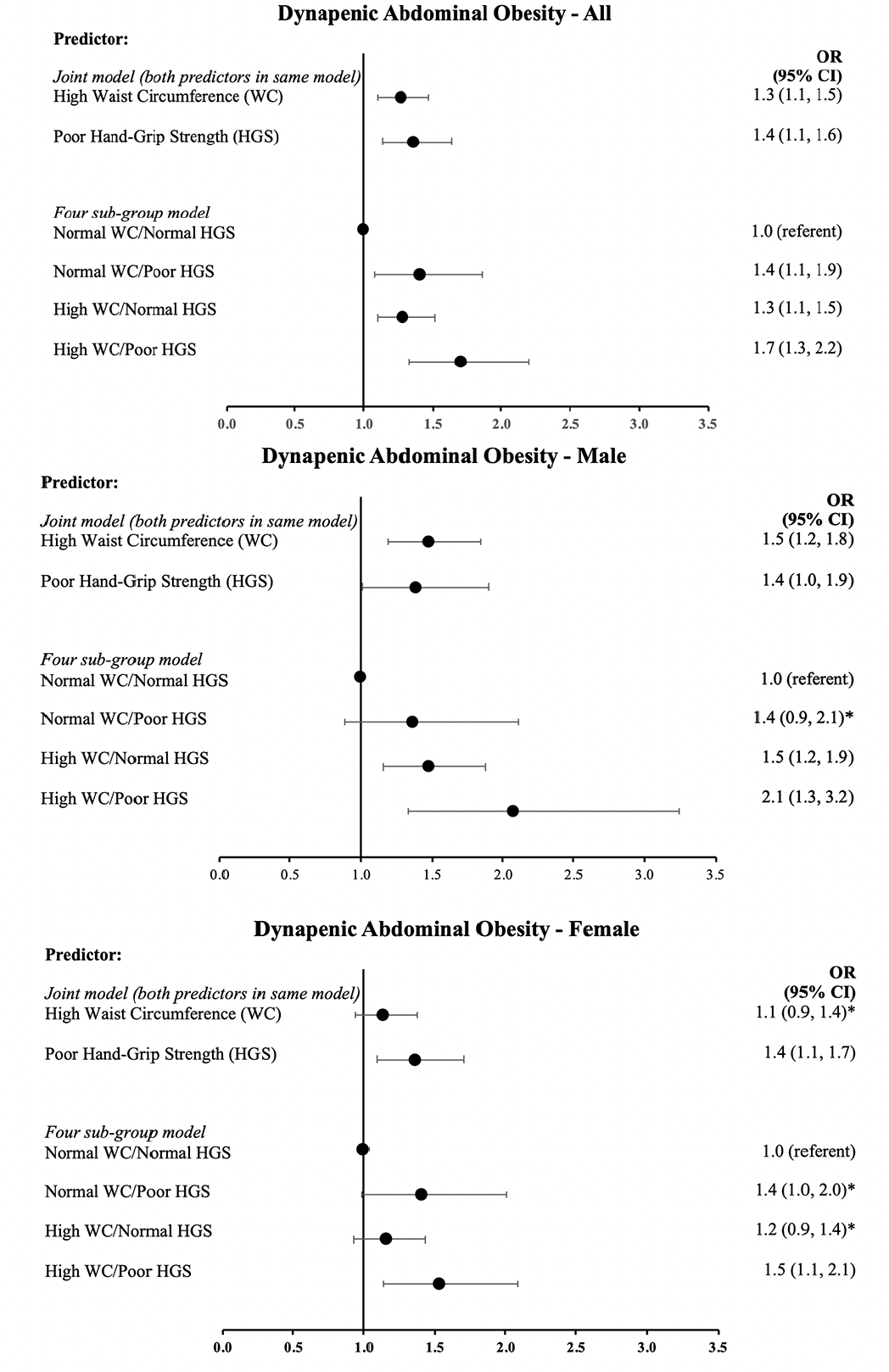
In the total study population, both high WC and low HGS were significantly and independently associated with falls (Fig 2a.) Thus, in a multivariate model containing both classifications, abdominal obesity (OR 1.3; 95% CI 1.1, 1.5) and dynapenia (OR 1.4; 95% 1.1, 1.6) were independently associated with falls incidence. All sub-groups of DAO had a higher OR of falling compared with the normal weight/non-dynapenic reference groups, independently of age and sex (Fig. 2a).The combination of both dynapenia and obesity (DAO) had the strongest association (OR 1.7; 95% CI 1.3, 2.2) with falls incidence (Fig 2a.) compared to those classified as normal weight (neither obese nor dynapenic).
Multiple logistic regression adjusted for age (b, c) and also sex (a). Dependent variable: Self-reported fall (yes/no). Joint-model independent variables: abdominal obesity expressed as high waist circumference (WC; >102cm M, >88cm F) and dynapenia expressed as poor hand-grip strength (HGS; <30kg M, <20kg F); the non-obese or non-dynapenic group was set as the reference. Four sub-group model: a categorical variable of dynapenic abdominal obesity (DAO); the normal WC/normal HGS group was set as the reference. Dynapenic Abdominal Obesity = WC (>102cm M, >88cm F) and HGS (<30kg M, <20kg F). Abbreviations: OR = odds ratio; CI = confidence interval. * Not significantly different from reference group.
Analysis by sex identified that the combination of abdominal obesity and dynapenia was associated with falls incidence in men (Fig. 2b). In contrast, both the joint-model analysis and four sub-group model confirmed that dynapenia rather than abdominal obesity was better associated falls in women (Fig. 2c). The OR for dynapenia and DAO in women was similar, however the dynapenic sub-group was not significant.
Discriminative ability of dynapenia, obesity and dynapenic obesity AUC analysis was used to determine how well continuous measures of dynapenia, obesity or definitions of dynapenic abdominal obesity predicted falls at an individual level. The receiver operating characteristic curves (ROC) demonstrated that the discriminative ability of dynapenia (AUC 0.51; 95% CI 0.49-0.53) or abdominal obesity was low (AUC 0.57; 95% CI 0.55-0.59) For the definition of DAO, AUC was also low (0.56; 95% CI 0.54-0.58) indicating poor discriminative ability. The AUC was similarly low when the group was divided by sex (data not shown).
EWGSOP2
As part of an exploratory analysis, we examined the relationship between the more recent EWGSOP2 consensus criteria of dynapenia (STS, HGS) (22) and falls. Using EWGSOP2 criteria (HGS <27kg (M), <16kg (F)), 7% (n=316) had low HGS (8% of women, 7% of men, p=0.076) and 14% had slow STS (<15s; 16% of women, 11% of men, p<0.001). Low HGS was not associated with falls in men or women. Sit-to-stand time predicted falls in women but this was not significant in men in either individual variable or joint model analysis (Table S1).
Discussion
In this observational cohort study of English adults aged 60-87 years, we found that individuals with DAO had a greater odds of falling compared with normal weight adults. However, a key finding of this study was the sex-specific relationship between abdominal obesity, dynapenia and falls: the combination of abdominal obesity and dynapenia, or DAO, was only predictive of falls in men. In contrast, dynapenia alone rather than abdominal obesity was a stronger predictor of falls in women.
In line with others (7, 8, 23), prevalence of dynapenic abdominal obesity was 9% in this cohort. This coexistence of dynapenia and abdominal obesity is concerning considering the aggravating (14-16) and potential synergistic effects of both phenotypes (24). In agreement with previous studies (10-12), we have demonstrated that DAO and its individual components are associated with falls incidence. Our novel findings that DAO is only predictive of falls in men with a lack of association observed between abdominal adiposity and falls in women, differ from the prospective study by Gadelha et al. [10] which found that the combination of dynapenia and abdominal obesity was associated with a greater risk of falling in older women. However, this study was small (n=201) and the individual phenotypes of dynapenia and abdominal obesity were not associated with falls. Other studies either did not consider sex separately (12) or looked at associations with falls risk rather than falls incidence (11).
There is reasonable correlation between upper and lower limb strength (25), thus potentially explaining the association between hand-grip strength and falls in both men and women. Additionally, hand-grip strength is associated with other factors (e.g. poor nutritional status (26)) which also associate with falls (2). However, this does not explain the discordant effects of abdominal obesity in men and women.
One possible explanation for our observed sexual dimorphism may relate to differences in fat distribution (and thus body shape) in men and women influencing an individual’s biomechanical movement. Menegoni et al. (27) found that greater BMI was associated with greater anterior-posterior instability in men and women whereas greater centre of pressure displacement and medio-lateral instability was only observed in men. The authors hypothesised that male (android) and female (gynoid) patterns of body fat distribution may explain this observation with an android shape characterised by greater mass/load over the hips and thus medio-lateral instability (27). Moreover, increased body mass, particularly abdominally, requires greater ankle torque to maintain stability (27, 28). Therefore, with regards to clinical intervention, although strength and balance training is currently recommended for falls prevention (1), carefully monitored weight management may provide another important consideration (29) given that abdominal obesity is an additional independent predictor of falls in men.
Finally, we explored and compared the definition of DAO using the latest consensus definitions of low muscle strength (22). The latest EWGSOP2 consensus suggests that dynapenia is sufficient to initiate clinical assessment and intervention (22). It is therefore interesting that low hand-grip strength using EWGSOP2 criteria did not predict falls in our study. In agreement with others (30, 31), our findings suggest that further research is required to understand how these cut-offs associate with functional outcomes. In addition, we observed sex-specific differences for sit-to-stand time suggesting that functional measures relate differently to falls incidence in men and women. These results suggest that, for the outcome of falls, hand-grip strength and sit-to-stand time may not be comparable surrogates as proposed (22).
The limitations of this study must be acknowledged. First, falls and fall-related injuries were self-reported and are subject to recall bias and thus may be inaccurate. Second, participants with incomplete measures were excluded and reasons for non-completion were not always available. Third, an age-range of 60-87 years may be considered a heterogenous group in relation to falls prevalence (32) and body composition (33, 34). However, a linear relationship was found between age and falls incidence, thus age was included as a covariate in our models. Fourth, analyses were exploratory and have not been corrected for multiple comparisons. Lastly, the effect of co-morbidities and other confounding factors (e.g. cognition, frailty, nutrition) requires further consideration. However, we did not include frailty as an independent variable as the Fried Frailty phenotype includes a measure of muscle strength and thus both are correlated.
Overall, dynapenia was associated with falls in men and women, whereas a link between abdominal obesity and falls was only evident in men. Consequently, a synergistic effect of abdominal obesity and dynapenia, DAO, and falls was only found in men. The use of these anthropometric and functional measures to identify patients at risk of falls is appealing due to their ease of clinical application and associations with adverse outcomes. A single cut-off approach has been utilised by numerous consensus committees (20, 22, 35) and further improves clinical acceptability and awareness. However, individual discrimination was low in this study suggesting that, in their current form, these measures may better serve as an adjunctive tool to clinical decision making (36). Of clinical relevance, our findings suggest that aside from targeting regular physical activity and strength training in later life to prevent dynapenia, weight maintenance and obesity prevention provide another potentially important public health intervention that may reduce the risk of falls in older people. This seems particularly relevant in older men considering our findings. The current challenge remains to find a way to operationalise a functionally-relevant definition of dynapenic abdominal obesity at an individual level and identify optimal treatment strategies.
Acknowledgements: The English Longitudinal Study of Ageing was developed by a team of researchers based at University College London, NatCen Social Research, the Institute for Fiscal Studies, the University of Manchester and the University of East Anglia. The data were collected by NatCen Social Research. The funding is currently provided by the National Institute on Aging in the US, and a consortium of UK government departments coordinated by the National Institute for Health Research. Funding has also been received by the Economic and Social Research Council.
Conflict of interest: None to declare.
Ethical standard: ELSA has received ethical approval from the South Central – Berkshire Research Ethics Committee (21/SC/0030, 22nd March 2021).
Funding: This work was supported by a studentship from the Medical Research Council (MRC) and Versus Arthritis as part of the Medical Research Council Versus Arthritis Centre for Integrated Research into Musculoskeletal Ageing (CIMA) [MR/R502182/1]. The MRC Versus Arthritis Centre for Integrated Research into Musculoskeletal Ageing is a collaboration between the Universities of Liverpool, Sheffield and Newcastle.
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. NICE. NICE guidelines [CG161] Falls in older people: assessing risk and prevention. Accessed December, 2020. https://www.nice.org.uk/guidance/cg161.
2. Masud T, Morris RO. Epidemiology of falls. Age Ageing 2001;30(suppl_4):3-7. https://doi.org/10.1093/ageing/30.suppl_4.3.
3. Cho B-Y, Seo D-C, Lin H-C, Lohrmann DK, Chomistek AK. BMI and central obesity with falls among community-dwelling older adults. Am J Prev Med 2018;54(4):e59-e66. https://doi.org/10.1016/j.amepre.2017.12.020.
4. Lin C-H, Liao K-C, Pu S-J, Chen Y-C, Liu M-S. Associated factors for falls among the community-dwelling older people assessed by annual geriatric health examinations. PLoS One 2011;6(4). https://doi.org/10.1371/journal.pone.0018976
5. Moreland JD, Richardson JA, Goldsmith CH, Clase CM. Muscle weakness and falls in older adults: a systematic review and meta-analysis. J Am Geriatr Soc 2004;52(7):1121-1129. https://doi.org/10.1111/j.1532-5415.2004.52310.x.
6. Karlsson MK, Ribom E, Nilsson J-Å, et al. Inferior physical performance tests in 10,998 men in the MrOS study is associated with recurrent falls. Age Ageing 2012;41(6):740-746. https://doi.org/10.1093/ageing/afs104.
7. da Silva Alexandre T, Scholes S, Santos JLF, de Oliveira Duarte YA, de Oliveira C. The combination of dynapenia and abdominal obesity as a risk factor for worse trajectories of IADL disability among older adults. Clin Nutr 2018;37(6):2045-2053. https://doi.org/10.1016/j.clnu.2017.09.018
8. Rossi AP, Urbani S, Fantin F, et al. Worsening disability and hospitalization risk in sarcopenic obese and dynapenic abdominal obese: a 5.5 years follow-up study in elderly men and women. Front Endocrinol 2020;11. https://doi.org/10.3389/fendo.2020.00314.
9. da Silva Alexandre T, Scholes S, Santos JF, de Oliveira Duarte YA, de Oliveira C. Dynapenic abdominal obesity increases mortality risk among English and Brazilian older adults: a 10-year follow-up of the ELSA and SABE studies. J Nutr Health Aging 2018;22(1):138-144. https://doi.org/10.1007/s12603-017-0966-4.
10. Gadelha AB, Neri SG, Vainshelboim B, Ferreira AP, Lima RM. Dynapenic abdominal obesity and the incidence of falls in older women: a prospective study. Aging Clin Exp Res 2019:1-8. https://doi.org/10.1007/s40520-019-01318-z.
11. Pereira JC, de Moraes Elias J, Neri SG, Gadelha AB, Lemos RR, Lima RM. Dynapenic abdominal obesity as a risk factor for falls in older women. Top Geriatr Rehabil 2019;35(2):149-155. https://doi.org/10.1097/TGR.0000000000000225.
12. de Oliveira Máximo R, Santos JLF, Perracini MR, de Oliveira C, de Oliveira Duarte YA, da Silva Alexandre T. Abdominal obesity, dynapenia and dynapenic-abdominal obesity as factors associated with falls. BJPT 2019;23(6):497-505. https://doi.org/10.1016/j.bjpt.2018.10.009.
13. World Health Organization. Waist circumference and waist-hip ratio: report of a WHO expert consultation, Geneva, 8-11 December 2008 2011.
14. de Carvalho DHT, Scholes S, Santos JLF, de Oliveira C, Alexandre TDS. Does abdominal obesity accelerate muscle strength decline in older adults? Evidence from the English Longitudinal Study of Ageing. J Gerontol A Biol Sci 2019;74(7):1105-1111. https://doi.org/10.1093/gerona/gly178.
15. Schrager MA, Metter EJ, Simonsick E, et al. Sarcopenic obesity and inflammation in the InCHIANTI study. J Appl Physiol (1985) 2007;102(3):919-25. https://doi.org/10.1152/japplphysiol.00627.2006.
16. Hubbard RE, Lang IA, Llewellyn DJ, Rockwood K. Frailty, body mass index, and abdominal obesity in older people. J Gerontol A Biol Sci Med Sci 2010;65(4):377-81. https://doi.org/10.1093/gerona/glp186.
17. Batsis JA, Villareal DT. Sarcopenic obesity in older adults: aetiology, epidemiology and treatment strategies. Nat Rev Endocrinol 2018;14(9):513-537. https://doi.org/10.1038/s41574-018-0062-9.
18. Steptoe A, Breeze E, Banks J, Nazroo J. Cohort profile: the English longitudinal study of ageing. Int J Epidemiol 2013;42(6):1640-1648. https://doi.org/10.1093/ije/dys168.
19. Dodds RM, Syddall HE, Cooper R, et al. Grip strength across the life course: normative data from twelve British studies. PLoS One 2014;9(12):e113637. https://doi.org/10.1371/journal.pone.0113637.
20. Cruz-Jentoft AJ, Baeyens JP, Bauer JM, et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing 2010;39(4):412-23. https://doi.org/10.1093/ageing/afq034.
21. NICE. Obesity: identification, assessment and management. NICE Guideline CG189. Accessed December, 2020. https://www.nice.org.uk/guidance/cg189/resources/obesity-identification-assessment-and-management-pdf-35109821097925.
22. Cruz-Jentoft AJ, Bahat G, Bauer J, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 2019;48(1):16-31. https://doi.org/10.1093/ageing/afy169.
23. Scott D, Chandrasekara SD, Laslett LL, Cicuttini F, Ebeling PR, Jones G. Associations of sarcopenic obesity and dynapenic obesity with bone mineral density and incident fractures over 5–10 years in community-dwelling older adults. Calcif Tissue Int 2016;99(1):30-42. https://doi.org/10.1007/s00223-016-0123-9.
24. Donini LM, Busetto L, Bauer JM, et al. Critical appraisal of Definitions and diagnostic criteria for sarcopenic obesity based on a systematic review. Clin Nutr 2019. https://doi.org/10.1016/j.clnu.2019.11.024.
25. Manini TM, Clark BC. Dynapenia and aging: an update. J Gerontol A Biol Sci Med Sci 2012;67(1):28-40. https://doi.org/10.1093/gerona/glr010.
26. Cederholm T, Jensen G, Correia MIT, et al. GLIM criteria for the diagnosis of malnutrition–A consensus report from the global clinical nutrition community. J Cachexia Sarcopenia Muscle 2019;10(1):207-217.
27. Menegoni F, Galli M, Tacchini E, Vismara L, Cavigioli M, Capodaglio P. Gender-specific effect of obesity on balance. Obesity 2009;17(10):1951-1956. https://doi.org/10.1038/oby.2009.82.
28. Corbeil P, Simoneau M, Rancourt D, Tremblay A, Teasdale N. Increased risk for falling associated with obesity: mathematical modeling of postural control. IEEE Trans Neural Syst Rehabil Eng 2001;9(2):126-36. https://doi.org/10.1109/7333.928572.
29. Matrangola SL, Madigan ML. Relative effects of weight loss and strength training on balance recovery. Med Sci Sports Exerc 2009;41(7):1488-1493. https://doi.org/10.1249/mss.0b013e31819bd4bd.
30. Petermann-Rocha F, Chen M, Gray SR, Ho FK, Pell JP, Celis-Morales C. New versus old guidelines for sarcopenia classification: What is the impact on prevalence and health outcomes? Age Ageing 2020;49(2):300-304. https://doi.org/10.1093/ageing/afz126.
31. Costanzo L, De Vincentis A, Di Iorio A, et al. Impact of Low Muscle Mass and Low Muscle Strength According to EWGSOP2 and EWGSOP1 in Community-Dwelling Older People. J Gerontol A Biol Sci Med Sci 2020;75(7):1324–1330. https://doi.org/10.1093/gerona/glaa063.
32. Gale CR, Cooper C, Aihie Sayer A. Prevalence and risk factors for falls in older men and women: The English Longitudinal Study of Ageing. Age Ageing 2016;45(6):789-794. https://doi.org/10.1093/ageing/afw129.
33. Goodpaster BH, Park SW, Harris TB, et al. The loss of skeletal muscle strength, mass, and quality in older adults: the health, aging and body composition study. J Gerontol A Biol Sci Med Sci 2006;61(10):1059-64. https://doi.org/10.1093/gerona/61.10.1059.
34. Delmonico MJ, Harris TB, Visser M, et al. Longitudinal study of muscle strength, quality, and adipose tissue infiltration. Am J Clin Nutr 2009;90(6):1579-85. https://doi.org/10.3945/ajcn.2009.28047.
35. Bhasin S, Travison TG, Manini TM, et al. Sarcopenia definition: the position statements of the sarcopenia definition and outcomes consortium. J Am Geriatr Soc 2020;68(7):1410-1418. https://doi.org/10.1111/jgs.16372.
36. Harvey NC, Odén A, Orwoll E, et al. Measures of Physical Performance and Muscle Strength as Predictors of Fracture Risk Independent of FRAX, Falls, and aBMD: A Meta-Analysis of the Osteoporotic Fractures in Men (MrOS) Study. J Bone Miner Res 2018;33(12):2150-2157. https://doi.org/10.1002/jbmr.3556.
37. Banks, J., Batty, G.D., Breedvelt, J.J.F., Coughlin, K., Crawford, R., Marmot, M., Nazroo, J., Oldfield, Z., Steel, N., Steptoe, A., Wood, Martin., Zaninotto, P. (2021) English Longitudinal Study of Ageing: Waves 0-9, 1998-2019 [data collection]. 36th Edition. UK Data Service. SN: 5050, http://doi.org/10.5255/UKDA-SN-5050-23