A.D. Jadczak1,2, M. Verma3, M. Headland3, G. Tucker2, R. Visvanathan1,2,4
1. Adelaide Geriatrics Training and Research with Aged Care (G-TRAC) Centre, Adelaide Medical School, Faculty of Health and Medical Sciences, University of Adelaide, Adelaide, SA, Australia; 2. National Health and Medical Research Council Centre of Research Excellence: Frailty Trans-Disciplinary Research to Achieve Healthy Ageing, University of Adelaide, Adelaide, SA, Australia; 3. Adelaide University Judo Club, Adelaide, SA, Australia; 4. Aged and Extended Care Services, The Queen Elizabeth Hospital, Central Adelaide Local Health Network, Adelaide, SA, Australia
Corresponding Author: Dr Agathe Daria Jadczak, PhD, Adelaide Geriatrics Training and Research with Aged Care (G-TRAC) Centre, Adelaide Medical School, Faculty of Health and Medical Sciences, University of Adelaide, Adelaide, South Australia, Australia. Basil Hetzel Institute for Translational Health Research, 37 Woodville Rd, Woodville South, South Australia 5011, Australia. Email: agathedaria.jadczak@adelaide.edu.au
Abstract
Objectives: This study aimed to explore the feasibility (including recruitment, safety and adherence) and the effects of a twice weekly supervised Judo-based exercise program over eight weeks on mobility, balance, physical performance, quality of life, fear of falling and physical activity (including by frailty status) in community-dwelling older people aged ≥65 years.
Design: Pre-post study.
Participants: A total of 17 participants (mean age 74.3±6.2; range 66-87 years; 76.5% female).
Intervention: A Judo-based exercise program conducted twice weekly for 60 minutes per session over eight weeks.
Measurements: Pre and post assessments included the Timed Up & Go (TUG); the Berg Balance Scale (BBS); the Short Physical Performance Battery (SPPB); the Short Form Health Survey-36 (SF-36); the Falls Efficiency Scale International (FES-I); and an ActivPal accelerometer to measure participants’ physical activity.
Results: Most participants had low (≤3) Charlson’s Comorbidity Index scores (n=17, 100%), were well nourished (n=16, 94.1%), not sarcopenic (n=16, 94.1%), and not cognitively impaired (n=13, 76.5%), anxious or depressed (n=14, 82.4%). Ten participants (58.8%) were non-frail and seven were pre-frail (41.2%). Significant improvements (p<0.05) were seen for mobility (TUG), balance (BBS) and physical performance (SPPB). Pre-frail participants showed greater improvement in mobility (TUG) than non-frail participants (p=0.020). No changes (p≥0.05) were seen in quality of life, fear of falling, or physical activity. Participants’ adherence (i.e., attending sessions) was high (i.e., ≥81.2%). No serious adverse events or withdrawals were reported.
Conclusion: Findings suggest that the eight week Judo-based exercise program can be delivered safely to older adults aged ≥65 years, including those at-risk of frailty, as long as there is close supervision with individualisation of the program in response to emergent health symptoms and the program is conducted on requisite Judo mats. This Judo-based exercise program is effective in improving physical function with potential to prevent falls and frailty risk.
Key words: Judo, older adults, frailty, falls, physical function.
Introduction
With globalisation, interest has increased in foreign cultures. Martial arts from Eastern countries have been adopted by many in the West for both their recreational value and health benefits. Increasingly, the possibility of improving the health of older people through supervised martial arts programs has become an area of interest among health professionals.
Tai Chi, for example, which has a focus on balance, has been shown to be beneficial in falls prevention (1). Judo, on the other hand, is a multi-component martial art that includes not only balance and strength training, but also teaches specific safe landing techniques (ukemi) that can be modified to teach older adults how to land safely when falling (2, 3). These safe landing techniques (ukemi) are unique to the sport of Judo and could potentially minimise harm and injury during falls (2, 3).
Falls are a common consequence of frailty, and improvements in parameters such as mobility, physical performance and balance have been associated with a reduction in frailty and falls risk in older people (4-7). Given the ageing population globally and the increasing prevalence of frailty and frailty-related consequences, such as falls (8), exploration of the health effects of martial arts, such as Judo, in older people is timely.
We conducted a scoping review (9) and found that there have been seven studies from Europe (i.e., Sweden, Italy, Spain and the Netherlands) focusing on community-dwelling older adults (mean age range 68.9 to 76 years) that have examined the effect of Judo on various health-related measures, including physical performance, gait speed, strength, quality of life, fear of falling, and flexibility. None of the studies had been conducted in Australia or reported on the effects of Judo in participants with varying frailty status.
Five of the studies were conducted over 10 to 16 weeks (sample size range 19 to 30) and significant improvements were noted in physical performance, gait speed, strength, fear of falling and flexibility (10-14) while two studies were of shorter durations (i.e. five to six weeks) with a similar sample size and found a reduction in fear of falling (15, 16). Only one study looked at the effects of Judo on balance in older adults (mean age 72±4.9 years) and showed improvements over 12 weeks (14), whilst no study to date had examined the effects of Judo on the Timed Up & Go (TUG), a mobility measure that assesses for falls and frailty risk in older adults (17, 18). The TUG includes gait speed, turning and sitting (17), providing more information than single-item measures such as gait speed.
The aims of the present study were to explore the feasibility (including recruitment, safety and adherence) and the effects of a twice weekly supervised Judo-based exercise program over eight weeks on mobility (including the TUG), balance, physical performance, quality of life, fear of falling and physical activity (including by frailty status) in community-dwelling older people aged ≥65 years.
Methods
The study was conducted between September and November 2021. Ethics approval was obtained from the University of Adelaide Human Research Ethics Committee (H-2021-078). The trial was registered with the Australian New Zealand Clinical Trials Registry (ACTRN12621001070820) prior to participant enrolment.
Participants
Participants were eligible if they were aged ≥65 years, community-dwelling, able to walk unsupported for everyday tasks, and had no diagnosed illnesses or conditions that would prevent them from participating in exercise. Participants were excluded if they had: a) been advised against physical exercise by their physician; b) a past history of congestive cardiac failure; c) experienced chest pain, dizziness or angina during exercise; d) uncontrolled high blood pressure; e) severe osteoporosis (T score <-2.5); f) atlantoaxial instability; g) or were unable to comply with the study protocol. The study was conducted at the Adelaide University Judo Club (AUJC) in Thebarton, Adelaide, South Australia.
Recruitment
Participants were recruited through the City of West Torrens (Local Government Council), which distributed flyers across newsletters, libraries and community groups. In addition, participants were recruited through social media, a newspaper advertisement, and flyers distributed across the AUJC network and the Centre of Research Excellence (CRE) in Frailty and Healthy Ageing, as well as the Basil Hetzel Institute for Translational Health Research in Adelaide, South Australia.
Individuals who expressed interest in the study were contacted via phone by the research team, who screened for eligibility and answered any questions. A participant information sheet (PIS), consent form, and a medical clearance template were then sent via post to eligible and interested individuals. Individuals were enrolled if they met all eligibility criteria and provided medical clearance from their general practitioner (GP), as well as written informed consent, prior to study start.
Judo-Based Exercise Intervention
The exercise program was based on Judo and included Judo-specific exercises such as break-falls (ukemi), a specific technique to learn how to land safely when falling, as well as a range of balance, strength and mobility tasks, which progressively increased in intensity and complexity over the course of the eight week study.
The Judo-based exercise program involved two supervised 60-minute group exercise sessions (max 10 participants per group) weekly for eight weeks, delivered by an experienced team of Judo coaches from the AUJC. The coaches included the Head Coach (6th degree black belt), the Technical Coach (4th degree black belt), and other 1st degree black belt Judo coaches, ensuring a 3:1 participant-instructor supervision. Both groups were supervised by the same team of Judo coaches.
The Judo-based exercise program was conducted on a sprung Judo tatami mat with softer landing mats added on top as needed. Each exercise session consisted of (1) a warm-up and practice getting up and down from the ground (10 min); (2) balance, strengthening and mobility exercises (10 min); (3) safe falling techniques (ukemi) (30 min); and (4) cool down exercises, including stretching and flexibility (10 min).
(1) Warm-up exercises included gentle, low impact limb and torso movements in various directions, including stretches up, down and side-to-side, as well as sequentially lowering to a seated position and rising again. The level of difficulty of the exercises increased over multiple sessions, commencing with the use of support – leaning on a chair or using two hands on the mat – progressing to no support.
(2) Balance, strength and mobility exercises included developing stable balance by learning to adopt a Judo stance. Participants stood with their feet shoulder width apart, gradually learning how to shift their weight when moving forwards, backwards and sideways, as well as when stepping up and down. Part way through the study, participants were encouraged to balance stably on one leg at a time. Strengthening the legs and core required slow, controlled, active sit-stands on sled chairs placed on the mat, which progressed to crawling across the mat, first on the stomach, later on the side or in a seated position.
(3) Safe falling techniques (ukemi) focussed on teaching head and neck control in the initial exercise sessions with the use of small beanbags held by the chin under the neck. This progressed to learning backward break-falls from seated positions through to standing positions, initially onto a landing mat, and then onto the Judo mat surface. Halfway through the program, participants began to learn side-falls onto landing mats from a simulated trip, as well as side-rolls from kneeling to automate a safe landing position. Exercises for front-falls onto forearms from knees and into a plank position were introduced mid-way through the program. By the final week, participants were introduced to forward-rolls over the shoulder differentiated between stable and unstable support during simulated fall exercises.
The Judo-specific details of the program are presented in Supplemental File 1.
Baseline Characteristic Assessments
Baseline data were collected one week prior to intervention start (week 0) and included information about the participants’ health, as well as socio-demographic information. The data recorded included number of falls over the past 12 months; participants’ mortality risk (Charlson Comorbidity Index – CCI) (19); risk of sarcopenia (SARC-F) (20); nutritional status (Mini Nutritional Assessment Short Form – MNA-SF) (21); cognition (Rapid Cognitive Screen – RCS) (22); anxiety and depression (Patient Health Questionnaire-4 – PHQ-4) (23); and grip strength (hand dynamometer) (24). Falls were defined as slipping, tripping, rolling and sliding resulting in the participant coming to rest inadvertently on the ground, floor or other lower level (25).
Frailty Status
Participants’ frailty status was assessed at baseline using the FRAIL Scale (26). The FRAIL Scale is a screening tool for frailty, which includes five yes-no questions about fatigue, resistance, ambulation, illness, and weight loss (26, 27). The FRAIL screen categorises adults into non-frail (0 indicators), pre-frail (1-2 indicators) and frail (≥3 indicators) based on the number of yes responses.
Intervention Satisfaction Assessment
Participants’ feedback and satisfaction on the Judo-based exercise program was sought using a post-intervention survey (Supplemental File 2).
Outcomes Assessment
The research team consisted of four research volunteers and two senior medical students who were trained by the lead researcher (i.e. exercise physiologist) on how to collected data prior to the study. All physical assessments were conducted by the lead researcher (i.e. exercise physiologist) and a senior medical student. The following assessments were conducted one week prior to intervention start (week 0) and one week after the intervention finished (week 9):
a) The Timed Up & Go (TUG) (17), a measure of mobility falls and frailty risk in older adults (17, 18). A cut-off score of ≥12 seconds was used to indicate limited mobility and a greater risk of falling (17).
b) The Berg Balance Scale (BBS) (28), a 14-item objective measure to assess falls risk and balance (static and dynamic) in older adults. Each item is scored between 0 (lowest level of function) and 4 (highest level of function). Possible scores range from 0 to 56 and risk is categorised as high falls risk (score 0-20), moderate falls risk (score 21-40), and low falls risk (score 41-56).
c) The Short Physical Performance Battery (SPPB) (29) combines the results of gait speed, chair stands and balance, and is used clinically to identify frailty risk (4). Possible scores range from 0 to 12, and physical limitation scores are categorised into severe physical limitations (score 0-3), moderate physical limitations (4-6), mild physical limitations (score 7-9), and minimal or no physical limitations (score 10-12) (29).
d) The Short Form Health Survey-36 (SF-36) (2), a self-reported health questionnaire containing 36 items measuring eight domains of physical and mental health. A scoring algorithm is used to convert the raw scores to a range between 0 and 100, with higher scores indicating a better quality of life.
e) The Falls Efficiency Scale International (FES-I) (30), a self-reported 16-item questionnaire assessing the fear of falling in older adults. The 16-items are scored between 1 (not at all concerned) and 4 (very concerned). Scores range from 16 to 64, and fear of falling is categorised into low concern (score 16-19), moderate concern (score 20-27), and high concern (score 28-64) of falling (31).
To reduce assessment time, the following questionnaires were handed/posted out to participants one week prior to their assessment: CCI, SARC-F, FRAIL Scale and satisfaction survey. Participants were instructed to complete the questionnaires/surveys within 48 hours prior to their assessment and bring the completed questionnaires to their appointment. The questionnaires were then checked for completion by the research team on assessment day.
Physical Activity Assessment
The ActivPal accelerometer is a thigh-worn device allowing for objective measure of physical activity in older adults (32, 33). The accelerometer was attached to a participant’s upper thigh with waterproof OPSITE dressing one week prior to intervention start (week 0) and again on the last day of the intervention (week 8). It was worn for seven days. Data extracted included average hours per day of lying/sitting, standing and stepping, as well as the number of steps and the number of sit-to-stand transitions, and the energy expenditure in the form of metabolic equivalents (METs). The average per day was calculated by summing up the data and dividing it by the days worn.
Compliance and Safety
Compliance and adverse events (AEs) were recorded by the research team at each exercise session using weekly compliance notes and adverse event forms. The type, duration, causality to the intervention, severity of symptom (i.e., mild, moderate, severe) and action (i.e., intervention unchanged, temporarily/permanent changed, or reduced\discontinued) were recorded for any physical symptoms experienced by the participants. The severity of a symptom was graded as follows: a) mild, if the symptom caused minimal discomfort and was easily tolerated by the participant; b) moderate, if the symptom was sufficiently discomforting; and c) severe, if the symptom was experienced as incapacitating. Participants were deemed to be compliant and were included in the analyses if they attended at least ≥70% of the exercise sessions (i.e., 11 out of 16 sessions).
Sample Size
This feasibility study aimed to include 20 participants (no age limit) to trial the eight week Judo-based exercise program. The results of the study will help to inform power calculations for a possible definitive randomised controlled trial.
Blinding
There was no blinding. Those collecting data were not involved in delivering the intervention.
Statistical Methods
Data were examined for normal distribution by inspecting histograms and using the Kolmogorov-Smirnov Test. Changes between pre and post data were analysed using the paired T-Test for normally distributed variables and the Wilcoxon signed rank test for not normally distributed variables. Differences between frailty group (i.e. non-frail and pre-frail) were analysed using the independent T-Test for normally distributed variables and the Mann-Whitney U Test for not normally distributed variables.
Descriptive data is presented as mean and standard deviation (SD). The statistical software SPSS version 25 (IBM Corporation. Armonk, NY) was used. The level of statistical significance was set at p<0.05.
Results
Recruitment
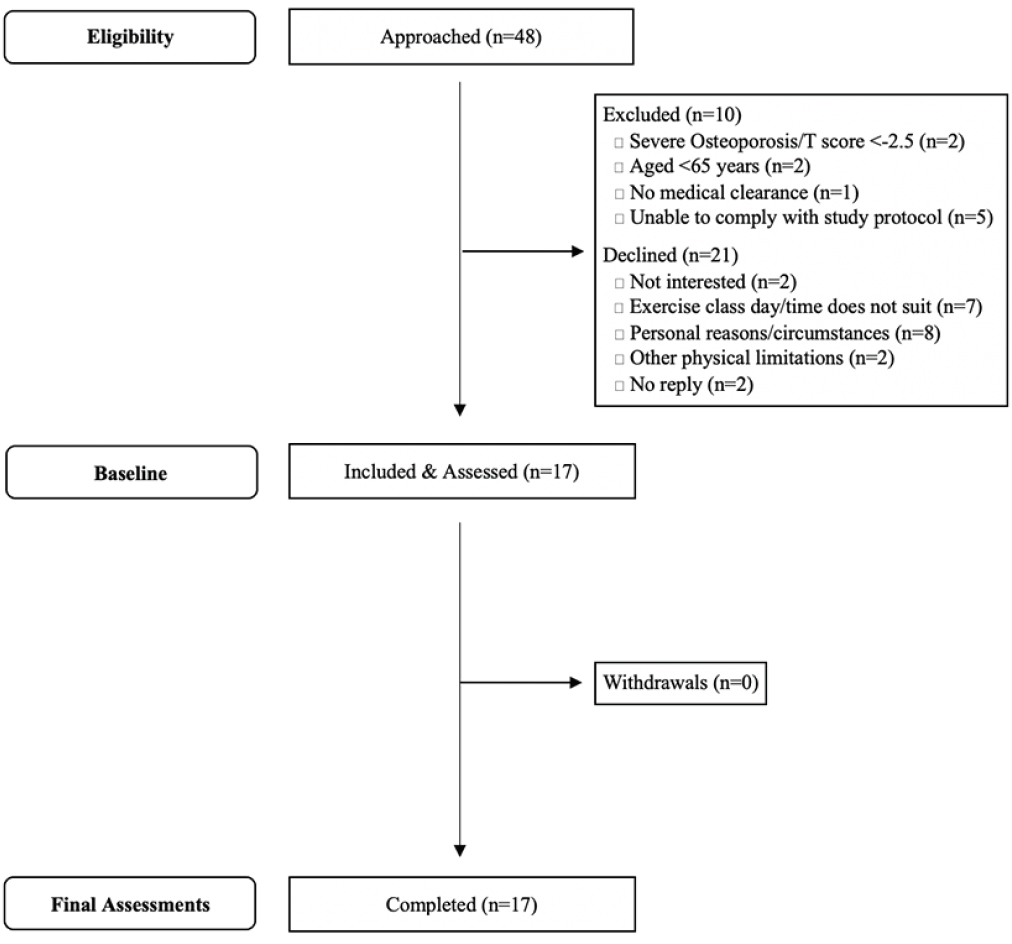
A total of 48 individuals expressed interest in the study (Figure 1). Out of the 48, 10 individuals were excluded due to not meeting the eligibility criteria, while 21 individuals opted out (43.8%): two were not interested, 17 had either personal reasons, other commitments or physical limitations that prevented them from participating, while two individuals did not respond.
Of the 48 interested individuals, almost half (n=23; 47.9%) became involved after a newspaper advertisement, with nine enrolling to participate (i.e. 39.1%). Promotion via the local council (The City of West Torrens) attracted eight individuals with three enrolling to participate (i.e. 37.5%). The five remaining study participants were recruited via word of mouth.
Participants
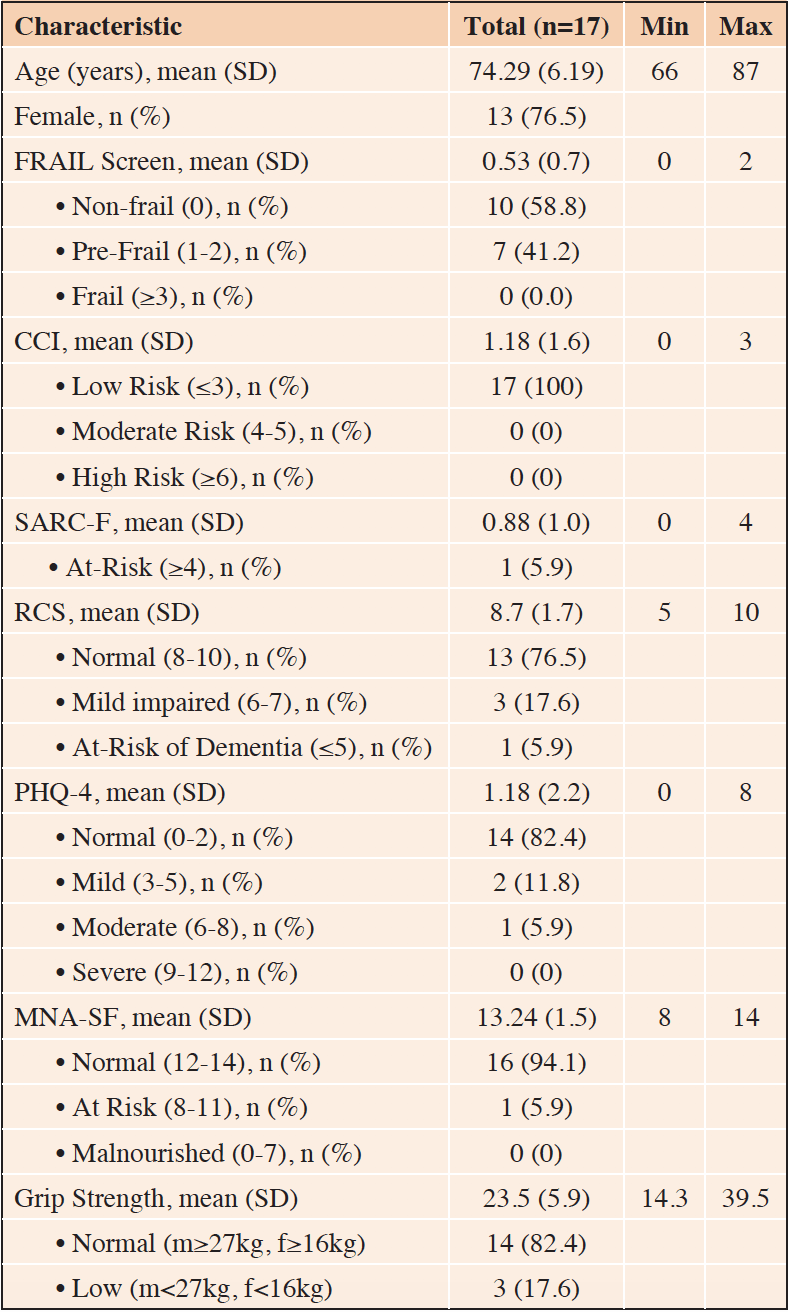
A total of 17 participants (mean age 74.3±6.2, range 66-87 years, 76.5% female) were included in the study. All participants had low (≤3) CCI scores (n=17, 100%) and the majority were well nourished (n=16, 94.1%), not sarcopenic (n=16, 94.1%), not cognitively impaired (n=13, 76.5%), anxious or depressed (n=14, 82.4%).
Ten participants (58.8%) were non-frail; seven were pre-frail (41.2%); and none were frail (Table 1).
IQR: interquartile range; CCI: Charlson Comorbidity Index; RCS: Rapid Cognitive Screen; PHQ-4: Patient Health Questionnaire-4; MNA-SF: Mini Nutritional Assessment Short Form, m:male; f:female
Withdrawals
There were no withdrawals.
Compliance
Compliance was high (≥81.2%), with all participants attending at least 13 out of 16 exercise sessions. Of these, seven participants attended 100% of the 16 exercise sessions, while ten participants missed between one and three exercise sessions (attendance range 93.7%-81.2%) over the eight week intervention.
Post-Intervention Evaluation
All participants reported being satisfied (11.8%, n=2) or very satisfied (88.2%, n=15) with the Judo-based exercise program.
Safety
Six non-serious AEs involving six participants were recorded, but only two were related to the study. Both were falls in week 5. One participant continued the study with no interruption. The other participant fell when attempting a backward-fall on a harder mat, which resulted in bruising and two physiotherapy appointments. This resulted in one missed and two reduced exercise sessions.
The four AEs unrelated to the study, which affected four different participants, included a muscle strain (week 5), an overnight fall (week 4), chest pain (week 4), and a car accident (week 7). The muscle strain resulted in three weeks (i.e., 6 sessions) of reduced exercises, whilst the chest pain led to one missed exercise session due to medical appointments. The overnight fall and car accident did not affect participation.
Intervention Modifications
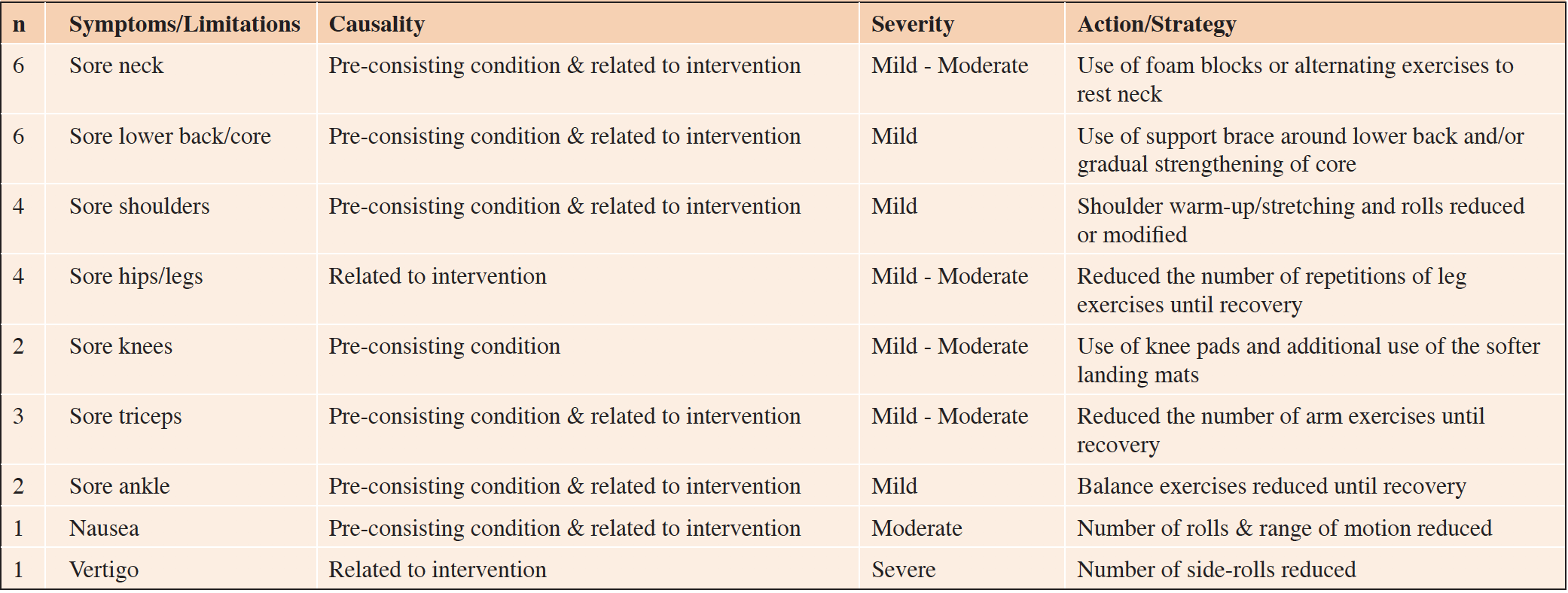
Four participants (23.5%) progressed through the Judo-based exercise program without experiencing any physical symptoms. Thirteen participants (76.5%) suffered from pre-existing conditions and reported mild to moderate muscle stiffness or soreness in either neck (n=6), lower back/core (n=6), shoulders (n=4), triceps (n=3), knees (n=2), hips/legs (n=4) or ankles (n=2). In addition, one participant suffered from nausea during the back-rolls, and another participant experienced severe vertigo after doing side-rolls repetitively.
Modifications tailored to relieve participants’ symptoms included using foam blocks (provided by AUJC) to allow participants’ necks to rest during the exercises. The range of motion during shoulder warm-ups was reduced for participants suffering from shoulder pain, and the amount of side and back-rolls limited for participants suffering from nausea or vertigo. Wearing knee pads or lower back support braces (supplied by participants) helped reduce the impact on participants’ knees and lower backs where necessary (Table 2).
n: number of participants
Outcome Measures
Timed Up & Go
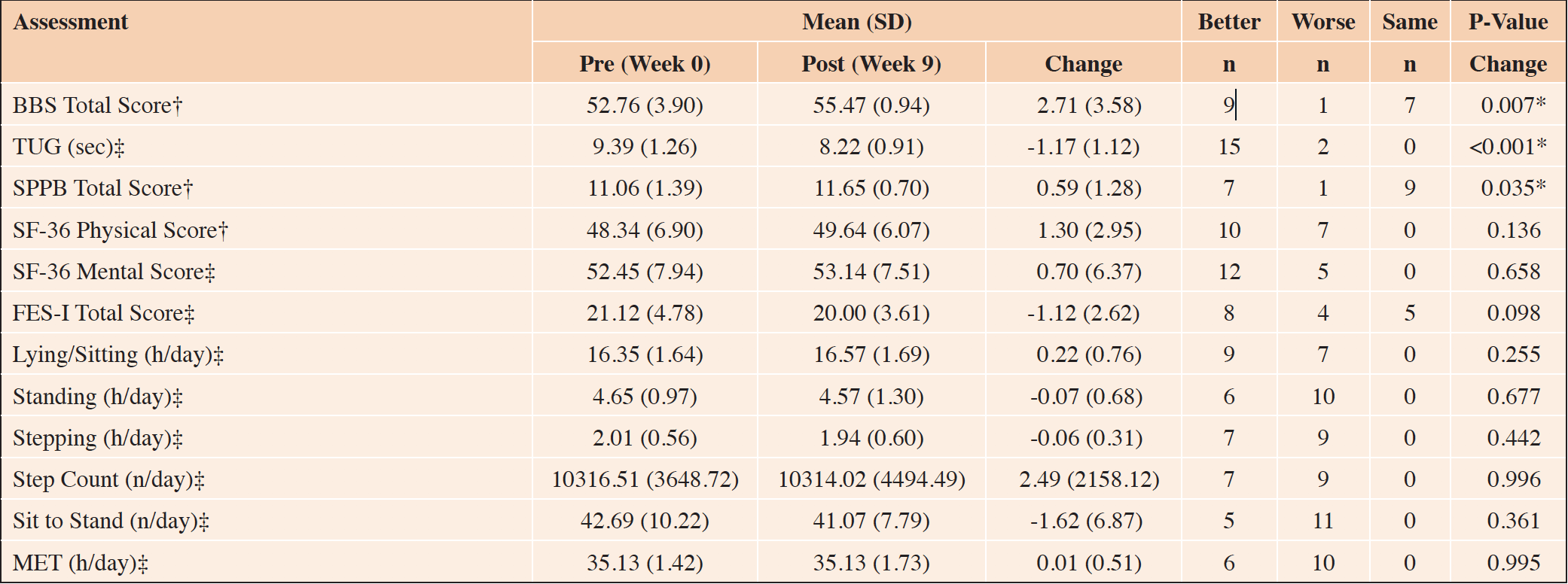
Pre-intervention, the majority of participants (n=16; 94.1%) exhibited good mobility (mean TUG 9.38±1.25 sec). The eight week Judo-based exercise program led to a significant positive change in TUG time (p<0.001) with the majority of participants (n=15, 88.2%) improving, while two participants worsened (Table 3).
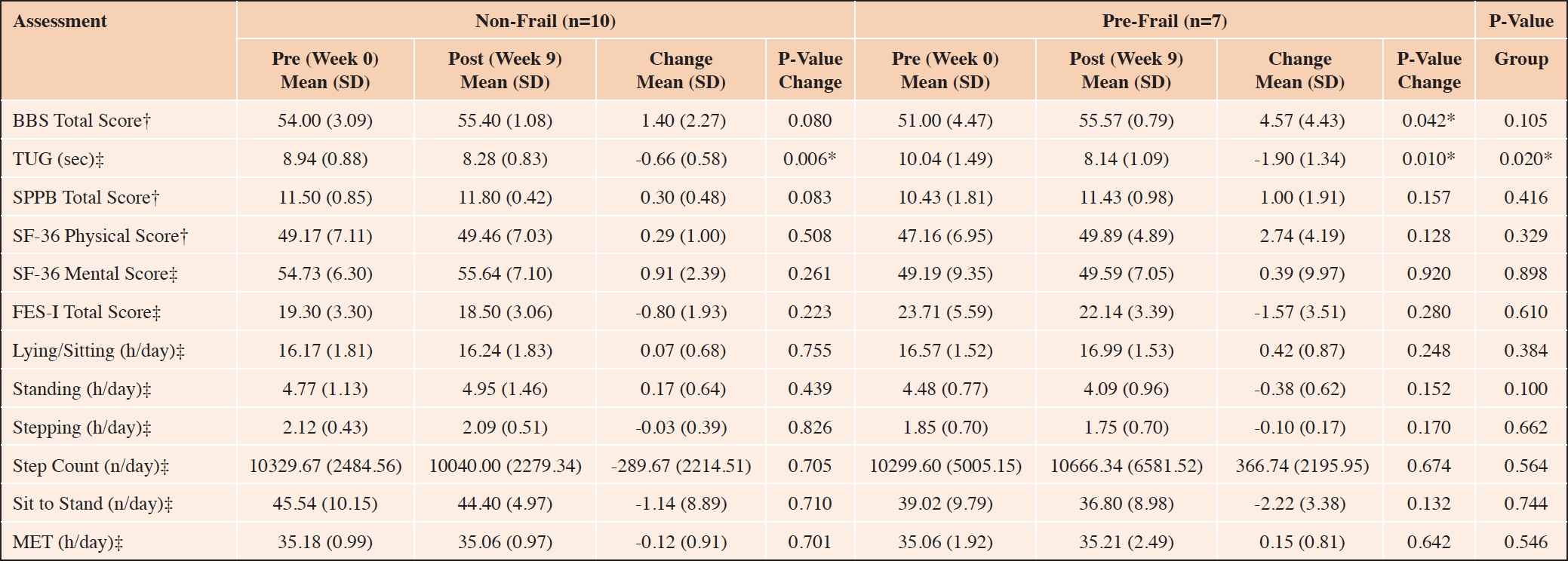
Both non-frail and pre-frail participants improved significantly (p<0.05), with greater improvement seen in pre-frail participants than in non-frail participants (p=0.020) (Table 4).
‡parametric test; †non parametric test; SD: standard deviation; BBS: Berg Balance Scale; n: number; h: hours, MET: one metabolic equivalent; SPPB: Short Physical Performance Battery; TUG: Timed Up and Go; FES-I: Falls Efficiency Scale International; SF-36: Short Form Health Survey-36; *significant p<0.05
‡parametric test; †non parametric test; BBS: Berg Balance Scale; TUG: Timed Up and Go; SPPB: Short Physical Performance Battery; FES-I: Falls Efficiency Scale International; SF-36: Short Form Health Survey-36; h: hours, MET: one metabolic equivalent; *significant p<0.05
Berg Balance Scale
All 17 participants (100.0%) had a low falls-risk, with BBS scores being high pre-intervention (mean 52.76±3.89). The eight week Judo-based exercise program led to a positive change in balance scores (p=0.007), with the majority of the participants (n=16, 94.1%) either improving (n=9) or remaining the same (n=8). Only one participant had a decrease in BBS total score (Table 3).
Pre-frail participants improved significantly in their BBS score post-intervention (p=0.042). However, this change was not significantly different to non-frail participants who did not significantly change following intervention (p=0.105) (Table 4).
Short Physical Performance Battery
SPPB total scores were high pre-intervention (mean score 11.06±1.39). The majority of the participants (n=15, 88.2%) exhibited either no or minimal physical limitations. At the end of the Judo-based exercise program, the majority of the participants (n=16, 94.1%) recorded a significant positive change in SPPB scores (p=0.035), either improving (n=7) or remaining the same (n=9). However, one participant recorded a decrease in the SPPB total score (Table 3).
No significant changes or differences were noted in the subgroups of pre-frail and non-frail participants (p≥0.05) (Table 4).
Quality of Life
Participants’ QoL scores ranged between 48.34±6.86 for the physical SF-36 component and 53.14±7.51 for the mental SF-36 component pre-intervention. Neither the mental nor the physical component changed for the total group (p≥0.05) and the sub groups of pre-frail and non-frail participants (p≥0.05) over the course of the study (Tables 3 and 4).
Fear of Falling
Participants’ fear of falling scores were low pre-intervention (mean 21.12±4.78), with the majority of participants (n=10, 58.8%) having little concern about falling. The exercise program did not lead to any significant changes in participants’ fear of falling scores for the total group (p≥0.05) and the sub groups of pre-frail and non-frail participants (p≥0.05) (Tables 3 and 4).
Physical Activity
Participants’ physical activity pre- and post-intervention, including lying/sitting, standing, stepping, as well as step count, sit-to-stand transitions, and energy expenditure (MET), did not result in lasting behavioural change. Pre- and post-values remained the same for the total group (p≥0.05), and the sub groups of pre-frail and non-frail participants (p≥0.05) (Tables 3 and 4).
Discussion
To the best of our knowledge, this is the first feasibility study reporting on the effects of a twice weekly Judo-based exercise program conducted over eight weeks on mobility (using the TUG) in older community-dwelling adults aged ≥65 years where over 40% of participants were pre-frail. Also, this is the first study originating from Australia. The findings suggest that the eight week Judo-based exercise program can be delivered to older adults, including those at-risk of frailty, as long as there is close supervision with intervention modifications in response to emergent symptoms or health issues. Given the improvements noted for mobility, balance and physical performance and given that measures such as the TUG and SPPB are cited in the literature as assessment methods for falls and frailty risk (4, 18), this intervention has the potential to reduce both falls and frailty risk in older community-dwelling adults, but this hypothesis requires further exploration through a randomised controlled trial.
Judo-based exercise programs have been shown to improve physical function parameters in older adults, including balance (14), physical performance (using the SPBB) (10, 14), gait speed (11) and muscle strength (12). Novel to our study was that an eight week Judo-based exercise program improved TUG time in older adults. Also, improvements in pre-frail participants were better than the improvements seen in non-frail participants. Impairment in TUG time has long been proposed as a method for screening for frailty risk (18). Therefore, this finding provides new evidence that Judo might be an effective intervention for frailty prevention for older people.
Adding to this, and similar to research recently reported elsewhere (10, 14), improvements to SPPB were noted in the majority (i.e., 9 out of 17) of participants. Everyone else, bar one, remained stable following the eight week program. Similar to TUG, SPPB is used clinically to identify frailty risk (4), and therefore interventions that can improve SPPB scores can be beneficial for frailty prevention.
In terms of Qol, fear of falling and physical activity, studies are sparse and results are mixed. Two studies examined QoL in older adults over 12 (14) to 16 (12) weeks and reported no significant changes, while there is some evidence to suggest that improvements in QoL may be noticed after longer interventions (i.e. 9 months, 3 session per week) when mixed-aged participants (aged 45 to 83 years) are investigated (2). Fear of falling improved in four (15, 16, 34, 35) out of six studies (12, 13, 15, 16, 34, 35) conducted in older adults with interventions ranging from five to 16 weeks, while physical activity was only studied in one study involving older adults showing improvements after twelve weeks (35). More research is needed to investigate the effects of Judo on health outcomes such as QoL, fear of falling, and physical activity.
A previous study has suggested that for Judo, the optimal program duration should consist of at least weekly sessions for 12 weeks (10), while another study suggests that motor skills and safe landing techniques can be learned by older adults (mean age 72±4.9 years) in a much shorter time of six to nine weeks of weekly sessions (14). Our study confirms that twice weekly sessions for eight weeks are feasible and we believe that this allows for effective progress including modification of intervention in response to participant symptoms or health issues. However, longer periods of participation may be recommended to realise health benefits, such as improved QoL (2) and bone mineral density (36-38).
Prior to this study, only one study, which included 28 healthy older adults (aged 60-88 years), has examined the safety and feasibility (i.e., recruitment and drop-out rates, time and recourses, and location) of a 45-60 minutes weekly Judo-based exercise program over 10-16 weeks (10). Each session was conducted with 7-10 participants and two Judo instructors (10). As in the present study, no serious adverse events were recorded (10). Our recommendation however is that close supervision is necessary when older adults with pre-existing health conditions, including pre-frailty, are participants. For example, in our study some pre-existing health conditions were exacerbated in some older participants, but modifications to their program enabled them to continue to participate. Also, many participants had health issues unrelated to the Judo program that required consideration also. Therefore, to ensure safe translation of Judo-based exercise programs into practice, Judo coaches need experience in both teaching Judo to a range of beginners and working with older adults.
Previous research also suggests that for older people, the local Judo club is a preferable location for an exercise program as Judo mats and Judo instructors are available at these locations (10). In our study, the Judo club proved essential in terms of providing time for the program and equipment. The permanent sprung Judo tatami mat surface proved essential for training and safety reasons when conducting safe-landing techniques (ukemi) with older adults.
No withdrawals were reported in this eight week study, and compliance rates were high (≥81.2%). Other studies that had included healthy older adults (aged 60 to 88 years) exercising once to twice per week over five to 16 weeks (10-12, 15) reported increasing dropout rates as the length of the program increased. Dropout rates of 10% were recorded during a five week intervention (15), 15% in a 15-16 week intervention (11, 12), and 25% in a 10-16 week intervention (10). Common reasons for leaving the program were medical (10, 11, 15) or personal (11) and unrelated to the intervention. Some participants were absent on the day of assessment (10) or had only attended sporadically (<75%) throughout the intervention (11, 12). More flexible program designs, experienced supervision to modify the program to participants’ health needs, and peer support for motivation (9, 39) could possibly counter poor adherence during lengthy interventions.
A limitation of this study was that it was conducted at only one Judo Club limiting the generalisability of the findings, and that it included only a small sample size with no control group. Further, safe landing techniques and falls rates were not assessed, and the study relied on the help of research volunteers and senior medical students due to budget constraints. A larger well-funded double-blinded randomized controlled trail across multiple clubs is needed to confirm the findings.
Conclusion
This Australian feasibility study examined for the first time the effects of an eight week Judo-based exercise program on mobility (using the TUG) in older community-dwelling adults aged ≥65 years. The findings suggest that a Judo-based exercise program can be delivered safely to older adults, including those at-risk of frailty, as long as some strategies to ensure participant safety are adhered to. Given the improvements noted for mobility, balance and physical performance, this Judo-based exercise program has the potential to reduce falls and frailty risk in older adults. However, a larger randomised controlled trial is needed to confirm these findings.
Acknowledgment: We would like to thank Melanie Pritchard, Michael Lynch, Véra Ada Daye and Laura Ayliffe for assisting with data collection. We would also like to thank Peter Ross, Michael Peachey, Janet Furler, Daniel Headland and William McPartland, our Judo study coaches, for conducting the centre-based exercise sessions. We would like to thank Udella Chan for assisting with recruitment and screening of participants, and Lesley Lewis and Véra Ada Daye for collecting weekly compliance data.
Funding: This research was funded by South Australian Government Office of Sport Recreation and Racing and the City of West Torrens, the National Health and Medical Research Council (Centre of Research Excellence Grant 1102208), and the Hospital Research Foundation. Open Access funding enabled and organized by CAUL and its Member Institutions.
Conflict of Interest: ADJ, GT and RV report no conflict of interest in relation to this project. MV and MH are Judo coaches at the AUJC who developed and delivered the eight week Judo-based exercise program. MV and MH were not involved in assessing participants or collecting data.
Ethical standards: Ethics approval was obtained from the University of Adelaide Human Research Ethics Committee (H-2021-078).
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. Huang Z-G, Feng Y-H, Li Y-H, Lv C-S. Systematic review and meta-analysis: Tai Chi for preventing falls in older adults. BMJ Open. 2017;7(2):e013661. doi: 10.1136/bmjopen-2016-013661.
2. Sakuyama N, Kamitani T, Ikumi A, Kida M, Kaneshiro Y, Akiyama K. Assessment of the efficacy and safety of a Judo exercise program in improving the quality of life among elderly patients. J Rural Med. 2021;16(4):229-235. doi: 10.2185/jrm.2021-008.
3. Kano J. Kodokan judo, 1st edn. Tokyo, JP: Kodansha International, 1986
4. Perracini MR, Mello M, de Oliveira Máximo R, et al. Diagnostic Accuracy of the Short Physical Performance Battery for Detecting Frailty in Older People. Phys Ther. 2020;100(1):90-98. doi: 10.1093/ptj/pzz154.
5. Panel on Prevention of Falls in Older Persons, American Geriatrics Society and British Geriatrics Society. Summary of the Updated American Geriatrics Society/British Geriatrics Society clinical practice guideline for prevention of falls in older persons. J Am Geriatr Soc. 2011;59(1):148-157. doi: 10.1111/j.1532-5415.2010.03234.x.
6. Falls: Assessment and Prevention of Falls in Older People. London: National Institute for Health and Care Excellence (NICE); 2013 Jun. PMID: 25506960.
7. Bloem BR, Steijns JA, Smits-Engelsman BC. An update on falls. Curr Opin Neurol. 2003;16(1):15-26. doi: 10.1097/01.wco.0000053580.70044.70.
8. Collard RM, Boter H, Schoevers RA, Oude Voshaar RC. Prevalence of frailty in community-dwelling older persons: a systematic review. JAGS. 2012;60(8):1487-1492. doi: 10.1111/j.1532-5415.2012.04054.x.
9. Chan U, Ayliffe L, Visvanathan R, Headland M, Verma M, Jadczak AD. Judo-Based Exercise Programs to Improve Health Outcomes in Middle-Aged and Older Adults: A Scoping Review. Geriatr Gerontol Int. 2023;23(3):163-178. doi: 10.1111/ggi.14553.
10. Arkkukangas M, Bååthe KS, Hamilton J, Ekholm A, Tonkonogi M. Feasibility of a novel Judo4Balance – fall preventive exercise programme targeting community-dwelling older adults. J Frailty Sarcopenia Falls. 2020;5(3):47-52. doi: 10.22540/JFSF-05-047.
11. Ciaccioni S, Capranica L, Forte R, Pesce C, Condello G. Effects of a 4-month judo program on gait performance in older adults. J Sports Med Phys Fitness. 2020;60(5):685-692. doi: 10.23736/S0022-4707.20.
12. Ciaccioni S, Capranica L, Forte R, Chaabene H, Pesce C, Condello G. Effects of a Judo Training on Functional Fitness, Anthropometric, and Psychological Variables in Old Novice Practitioners. J Aging Phys Act. 2019;27(4):831-842. doi: 10.1123/japa.2018-0341.
13. Ciaccioni S, Pesce C, Capranica L, Condello G. Effects of a judo training program on falling performance, fear of falling and exercise motivation in older novice judoka. Ido Mov Culture. J Martial Arts Anthrop. 2021;21(3):9-17. doi: 10.14589/ido.21.3.2.
14. Arkkukangas M, Strömqvist Bååthe K, Ekholm A, Tonkonogi M. High Challenge Exercise and Learning Safe Landing Strategies among Community-Dwelling Older Adults: A Randomized Controlled Trial. Int J Environ Res Public Health. 2022;19(12):7370. doi: 10.3390/ijerph19127370.
15. Groen BE, Smulders E, de Kam D, Duysens J, Weerdesteyn V. Martial arts fall training to prevent hip fractures in the elderly. Osteoporos Int.2010;21(2):215-221. doi: 10.1007/s00198-009-0934-x.
16. Campos-Mesa MCD-A, Óscar Toronjo-Hornillo, Luis Castañeda-Vázquez, Carolina. The Effect of Adapted Utilitarian Judo, as an Educational Innovation, on Fear-of-Falling Syndrome. Sustainability. 2020;12(10):4096. doi.org/10.3390/su12104096.
17. Podsiadlo D, Richardson S. The timed ‘Up & Go’: a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc. 1991;39(2):142-148. doi: 10.1111/j.1532-5415.1991.tb01616.x.
18. Savva GM, Donoghue OA, Horgan F, O’Regan C, Cronin H, Kenny RA. Using timed up-and-go to identify frail members of the older population. J Gerontol A Biol Sci Med Sci. 2013;68(4):441-446. doi: 10.1093/gerona/gls190.
19. Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373-383. doi: 10.1016/0021-9681(87)90171-8.
20. Woo J, Leung J, Morley JE. Validating the SARC-F: a suitable community screening tool for sarcopenia? J Am Med Dir Assoc. 2014;15(9):630-634.
21. Guigoz Y, Lauque S, Vellas BJ. Identifying the elderly at risk for malnutrition. The Mini Nutritional Assessment. Clin Geriatr Med. 2002;18(4):737-757. doi: 10.1016/j.jamda.2014.04.021.
22. Malmstrom TK, Voss VB, Cruz-Oliver DM, Cummings-Vaughn LA, Tumosa N, Grossberg GT, et al. The Rapid Cognitive Screen (RCS): A Point-of-Care Screening for Dementia and Mild Cognitive Impairment. J Nutr Health Aging. 2015;19(7):741-744. doi: 10.1007/s12603-015-0564-2.
23. Kroenke K, Spitzer RL, Williams JB, Lowe B. An ultra-brief screening scale for anxiety and depression: the PHQ-4. Psychosomatics. 2009;50(6):613-621. doi: 10.1176/appi.psy.50.6.613.
24. Cruz-Jentoft AJ, Bahat G, Bauer J, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing. 2019;48(1):16-31. doi: 10.1093/ageing/afy169.
25. World Health Organisation. 2007 WHO global report on falls prevention in older age.
26. Morley JE, Vellas B, van Kan GA, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013;14(6):392-397. doi: 10.1016/j.jamda.2013.03.022.
27. Woo J, Leung J, Morley JE. Comparison of frailty indicators based on clinical phenotype and the multiple deficit approach in predicting mortality and physical limitation. J Am Geriatr Soc. 2012;60(8):1478-1486. doi: 10.1111/j.1532-5415.2012.04074.x.
28. Berg KO, Maki BE, Williams JI, Holliday PJ, Wood-Dauphinee SL. Clinical and laboratory measures of postural balance in an elderly population. Arch Phys Med Rehabil. 1992;73(11):1073-1080.
29. Guralnik JM, Simonsick EM, Ferrucci L, Glynn RJ, Berkman LF, Blazer DG. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol. 1994;49(2):M85-94. doi: 10.1093/geronj/49.2.m85.
30. Yardley L, Beyer N, Hauer K, Kempen G, Piot-Ziegler C, Todd C. Development and initial validation of the Falls Efficacy Scale-International (FES-I). Age Ageing. 2005;34(6):614-619. doi: 10.1093/ageing/afi196.
31. Delbaere K, Close JCT, Mikolaizak AS, Sachdev PS, Brodaty H, Lord SR. The Falls Efficacy Scale International (FES-I). A comprehensive longitudinal validation study. Age Ageing. 2010;39(2):210-216. doi: 10.1093/ageing/afp225.
32. Stevens ML, Gupta N, Inan Eroglu E, Crowley PJ, Eroglu B, Bauman A, et al. Thigh-worn accelerometry for measuring movement and posture across the 24-hour cycle: a scoping review and expert statement. BMJ Open Sport Exerc Med. 2020;6(1):e000874. doi: 10.1136/bmjsem-2020-000874.
33. Blackwood J, Suzuki R, Webster N, Karczewski H, Ziccardi T, Shah S. Use of activPAL to Measure Physical Activity in Community-Dwelling Older Adults: A Systematic Review. Arch Rehabil Res Clin Trans. 2022;4(2):100190. doi: 10.1016/j.arrct.2022.100190.
34. Toronjo-Hornillo L, Castañeda-Vázquez C, Campos-Mesa MDC, et al. Effects of the Application of a Program of Adapted Utilitarian Judo (JUA) on the Fear of Falling Syndrome (FOF) for the Health Sustainability of the Elderly Population. Int J Environ Res Public Health. 2018;15(11):2526. doi: 10.3390/ijerph15112526.
35. Arkkukangas M, Karin Strömqvist B, Ekholm A, Tonkonogi M. High Challenge Exercise and Learning Safe Landing Strategies among Community-Dwelling Older Adults: A Randomized Controlled Trial. Int J Environ Res Public Health. 2022;19(12):7370. doi: 10.3390/ijerph19127370.
36. Borba-Pinheiro CJ, Figueiredo NMA, Carvalho MCGA, et al. Adapted Judo training on bone-variables in postmenopausal women in pharmacological treatment. Sport Sci Health. 2012;8(2):87-93. doi:10.1007/s11332-012-0134-5.
37. Borba-Pinheiro CJ, de Alencar Carvalho MCG, da Silva NSL, Drigo AJ, Bezerra JCP, Dantas EHM. Bone density, balance and quality of life of postmenopausal women taking alendronate participating in different physical activity programs. Ther Adv Musculoskelet Dis. 2010;2(4):175-185. doi: 10.1177/1759720X10374677.
38. Borba-Pinheiro C, Carvalho MC, Drigo A, et al. Combining Adapted Judo Training and pharmacological treatment to improve Bone Mineral Density on postmenopausal women: A two years study. Archives of Budo. 2013;9:81-88.
39. Thomas GN, Macfarlane DJ, Guo B, et al. Health promotion in older Chinese: a 12-month cluster randomized controlled trial of pedometry and «peer support». Med Sci Sports Exerc. 2012;44(6):1157-1166. doi: 10.1249/mss.0b013e318244314a.
The Author(s) 20223