R. McGrath1, P.J. Carson2, D.A. Jurivich3
1. Department of Health, Nutrition, and Exercise Sciences, North Dakota State University, Fargo, ND, USA;
2. Department of Public Health, North Dakota State University, Fargo, ND, USA; 3. Department of Geriatrics, University of North Dakota, Grand Forks, ND, USA
Corresponding Author: Ryan McGrath, Department of Health, Nutrition, and Exercise Sciences, North Dakota State University, NDSU Dept. 2620, PO Box 6050, Fargo, ND 58108-6050, Phone: 701-231-7474, Fax: 701-231-8872, Email: ryan.mcgrath@ndsu.edu
J Frailty Aging 2021;10(3)301-302
Published online January 6, 2020, http://dx.doi.org/10.14283/jfa.2020.73
Dear Editor,
SARS-CoV-2, the cause of COVID-19, remains a novel infectious virus that has led to millions of cases globally. While COVID-19 infection and death prevention remain a top public health priority, post-hospitalization COVID-19 recovery is also important and emerging in adults surviving infection. For example, persons that survived a COVID-19 hospitalization have persisting mobility impairments and morbidities several months post-hospitalization (1). Given that the initial months after a critical illness hospitalization are crucial for functional recovery, monitoring physical functioning and related biomarkers after discharge from a COVID-19 hospitalization could be vital for functional recovery, and the proper deployment of relevant interventions.
The pathophysiology related to functional recovery after a COVID-19 hospitalization may provide insights into improving the recovery process. For example, respiratory virus infections, such as COVID-19, trigger inflammatory responses at both the site of the infection and systemically (2). “Cytokine storms” have been observed in those with COVID-19 infections, which is linked to the same tissue damage and organ system failures that contributes to poor physical functioning (3). The hyperinflammatory states seen in COVID-19 patients are related to the inflammaging that leads to functional declines during aging, even in younger individuals (4). Interleukin-6 is a prognosticator in patients with COVID-19 (5), and is likewise an important contributor to declines in muscle function (6). Thus, the inflammatory responses observed in middle-aged and older adults with COVID-19, especially after hospitalization, could predict functional trajectories.
Clinical assessments of physical functioning help to identify the onset and progression of the disabling cascade (7). Although physical performance assessments such as gait speed may provide useful information regarding functional recovery from COVID-19 after hospitalization, these assessments have limitations because they require full body movements. Alternatively, muscle function assessments present organ level insights for the initial stages of physical function deficits. Muscle dysfunction precedes the physical performance limitations that lead to mobility impairments and morbidities such as sarcopenia (8).
Handgrip strength is a convenient assessment of strength capacity and reliable measure of muscle function that requires patients to squeeze a relatively inexpensive isometric dynamometer with maximal effort for a short duration (e.g., 3-5 seconds). As such, handgrip strength measurements are commonly used in clinical and research settings to examine muscle function. However, protocols for handgrip strength focus exclusively on maximal strength, and other muscle function characteristics that may better elucidate muscle dysfunction remain overlooked.
Utilizing digital handgrip dynamometers and attaching a triaxial accelerometer on the top of a dynamometer may help in evaluating the additional aspects of muscle function that are not otherwise ascertained with traditional handgrip dynamometers (9). For example, digital handgrip dynamometry and accelerometry have the ability to not only measure maximal strength, but also strength asymmetry, explosiveness, coordination, force steadiness, fatigability, and muscle contraction induced tremoring. Some of these aspects, such as fatigability, could similarly extend into the use of handgrip dynamometers for the concept of resilience, which may be important for COVID-19 survival and recovery. Utilizing digital handgrip dynamometry and accelerometry also maintains procedural ease and overall test inclusiveness for persons recovering from a COVID-19 hospitalization.
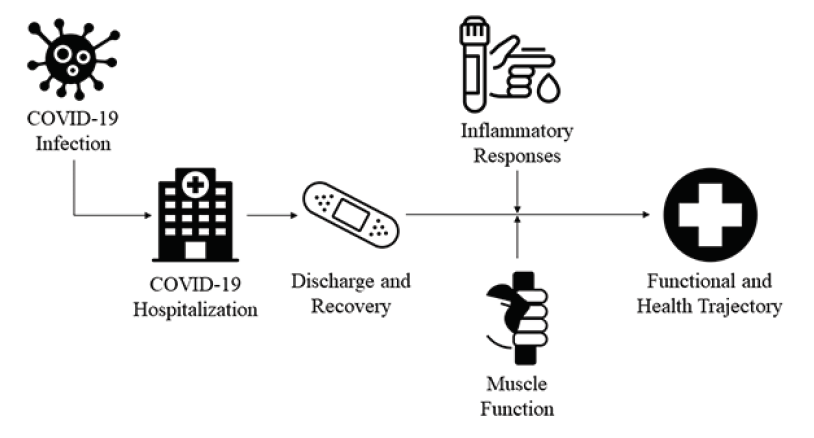
Figure 1
Conceptual Model for Monitoring Inflammatory Responses and Muscle Function for Predicting Functional Recovery After COVID-19 Hospitalization
Figure 1 presents a conceptual model for observing inflammatory responses and muscle function to predict functional recovery in persons recovering from a COVID-19 hospitalization. Overall, inflammation is an important biomarker for muscle function (10), and inflammatory responses occurring during COVID-19 infections could be linked to diminished physical functioning after COVID-19 recovery. Very little is known about how serum biomarkers and the several attributes of muscle function could be impacted after a COVID-19 hospitalization. Inflammatory responses occurring during COVID-19 critical illness hospitalizations that influence functional recovery could be worse than non-COVID-19 illness hospitalizations. Monitoring inflammatory responses and physical functioning in patients that are recovering from COVID-19 at discharge and intermittently thereafter may help to predict their functional trajectories and allow for timely interventions that foster recovery. Therefore, healthcare providers should strongly consider measuring inflammatory responses and physical functioning in COVID-19 patients sustaining a hospitalization if they are not already, and research efforts may likewise provide additional insights. Similar work may also have generalizability to other relevant hospitalizations.
Given the ongoing novelty of COVID-19, examining inflammatory responses and physical functioning is important for patients recovering from COVID-19 not only regain independent living, but also provide new information into the recovery process. While COVID-19 prevention and treatment are still of the utmost importance, surveilling the health of the growing number of persons recovering from a COVID-19 hospitalization will also emerge as a necessary implication.
Conflict of interest: No conflicts of interest.
References
1. Garrigues E, Janvier P, Kherabi Y, et al. Post-discharge persistent symptoms and health-related quality of life after hospitalization for COVID-19. J Infect. 2020;81(6):e4-e6. doi:10.1016/j.jinf.2020.08.029.
2. Dutta A, Das A, Kondziella D, Stachowiak MK. Bioenergy Crisis in Coronavirus Diseases? Brain Sci. 2020;10(5):277. Published 2020 May 2. doi:10.3390/brainsci10050277.
3. Ragab D, Salah Eldin H, Taeimah M, Khattab R, Salem R. The COVID-19 Cytokine Storm; What We Know So Far. Front Immunol. 2020;11:1446. Published 2020 Jun 16. doi:10.3389/fimmu.2020.01446.
4. Bektas A, Schurman SH, Franceschi C, Ferrucci L. A public health perspective of aging: do hyper-inflammatory syndromes such as COVID-19, SARS, ARDS, cytokine storm syndrome, and post-ICU syndrome accelerate short- and long-term inflammaging?. Immun Ageing. 2020;17:23. Published 2020 Aug 24. doi:10.1186/s12979-020-00196-8.
5. Grifoni E, Valoriani A, Cei F, et al. Interleukin-6 as prognosticator in patients with COVID-19. J Infect. 2020;81(3):452-482. doi:10.1016/j.jinf.2020.06.008.
6. Grosicki GJ, Barrett BB, Englund DA, et al. Circulating Interleukin-6 Is Associated with Skeletal Muscle Strength, Quality, and Functional Adaptation with Exercise Training in Mobility-Limited Older Adults. J Frailty Aging. 2020;9(1):57-63. doi:10.14283/jfa.2019.30.
7. Patrizio E, Calvani R, Marzetti E, Cesari M. Physical Functional Assessment in Older Adults. J Frailty Aging. 2020 (In Press). https://doi.org/10.14283/jfa.2020.61.
8. Crosigani S, Sedini C, Calvani R, et al. Sarcopenia in Primary Care: Screening, Diagnosis, Management. J Frailty Aging. 2020 (In Press). https://doi.org/10.14283/jfa.2020.63.
9. Mahoney S, Klawitter L, Hackney KJ, et al. Examining Additional Aspects of Muscle Function with a Digital Handgrip Dynamometer and Accelerometer in Older Adults: A Pilot Study. Geriatrics (Basel). 2020;5(4):86. Published 2020 Oct 31. doi:10.3390/geriatrics5040086.
10. Rodriguez-Mañas L, Araujo de Carvalho I, Bhasin S, et al. ICFSR Task Force Perspective on Biomarkers for Sarcopenia and Frailty. J Frailty Aging. 2020;9(1):4-8. doi:10.14283/jfa.2019.32.
