C.P. Launay1,2, L. Cooper-Brown2,3, V. Ivensky2,4, O. Beauchet1,2,5,6
1. Department of Medicine, Division of Geriatric Medicine, Sir Mortimer B. Davis – Jewish General Hospital and Lady Davis Institute for Medical Research, McGill University, Montreal, Quebec, Canada; 2. Centre of Excellence on Longevity of McGill integrated University Health and social services Network, Quebec, Canada; 3. Faculty of Medicine, McGill University, Montreal, Quebec, Canada; 4. Faculty of Medicine, University of Montreal, Montreal, Quebec, Canada; 5. Dr. Joseph Kaufmann Chair in Geriatric Medicine, Faculty of Medicine, McGill University, Montreal, Quebec, Canada; 6. Lee Kong Chian School of Medicine, Nanyang Technological University, Singapore
Corresponding Author: Olivier Beauchet, MD, PhD; Department of Medicine, Division of Geriatric Medicine, Sir Mortimer B. Davis – Jewish General Hospital, McGill University, 3755 chemin de la Côte-Sainte-Catherine, Montréal, QC H3T 1E2, Canada; E-mail: olivier.beauchet@mcgill.ca; Phone: (+1) 514-340-8222, #24741; Fax: (+1) 514-340-7547
J Frailty Aging 2020;
Published online December 22, 2020, http://dx.doi.org/10.14283/jfa.2020.69
Dear Editor,
Recently, Aubertin-Leheurdre & Rolland underscored issues and challenges related to the insufficient physical activity levels observed in the frail older population due to social distancing during the Coronavirus disease 2019 (COVID-19) pandemic (1). Social distancing is an effective intervention to limit the spread of COVID-19 (2). However, for older community dwellers social distancing implies homebound which may lead to a decline in physical activity, increased gait and balance disorders, cardiovascular disease burden and morality risk (1, 3, 4).
Frailty refers to a condition of vulnerability to physical and psychological stressors that exposes individuals to incident adverse health events, disabilities and death (5-7). There are two frailty phenotypes: physical and mental (6, 7). We suggested that frailty phenotypes may confer distinct risks for adverse outcomes to homebound older community dwellers. To explore this research hypothesis, there is a need to first gather information about homebound older adults’ physical and mental frailty phenotypes at the onset of confinement. Montreal (Quebec, Canada) is an urban area that is particularly affected by the COVID-19 pandemic, being, as of May 2020, the city with the highest number of confirmed COVID-19 cases in Canada (8). The confinement of Montreal’s older adults will be therefore lasting longer than initially anticipated.
A short assessment tool, known as “Évaluation SOcio-GÉRiatrique” (ESOGER), for Montreal’s older community-dwelling population has been designed in March 2020. ESOGER allows to screen both physical and mental frailty. The objective of the present study is to describe the clinical characteristics and frailty phenotype of Montreal’s older community dwellers, assessed with ESOGER after one month of being homebound.
Between April 20 and May 08, 2020, 879 older community dwellers were recruited to participate in this cross-sectional study. Selection criteria were: age ≥70 years, being homebound, understanding French and/or English and agreeing to participate in the study. ESOGER is a clinical assessment consisting of a digital questionnaire that includes close-ended questions exploring five complementary subdomains, including: 1) COVID-19 clinical symptomatology (i.e., fever ≥38°C/100F, cough, shortness of breath and other symptoms); 2) a frailty assessment performed using the 6-item brief geriatric assessment (BGA), 3) psychological stress using a verbal analogue scale (VAS) of anxiety ranging from 0 (i.e., no anxiety) to 10 (i.e., severe anxiety) (9). ESOGER can be filled out by health and social professionals, as well as by trained volunteers, through a phone call with older community dwellers or their caregivers. Participants were separated into 4 groups based on their frailty phenotype as per the 6-item BGA: no frailty, physical frailty (i.e., use of a walking aid), mental frailty (i.e., temporal disorientation associated with anxiety), and a combination of physical and mental frailty. Participants’ characteristics were summarized using frequencies and percentages. Between-group comparisons were performed using Chi-squared tests. P-values less than 0.001 were considered statistically significant because of multiple comparisons (n = 42). All statistics were performed using SPSS (version 24.0; SPSS, Inc., Chicago, IL). The study was approved by the Ethics Committee Of thé Jewish General Hospital (Montreal, Quebec, Canada).
The overall prevalence of frailty was 65.0%; the most prevalent type was physical frailty 38.3%, whereas the prevalence of mental frailty was 12.5%, and that of both frailties combined was 14.1% (Table 1). Participants identified as physically frail were older, used home support, and experienced polypharmacy at a higher rate than those with no frailty (P≤0.001) and those with mental frailty (P≤0.001). Participants combining both types of frailty took more medications compared to those with no frailty (P≤0.001) and had home support more often than those with mental frailty only (P≤0.001). There were no significant differences between groups for the other characteristics.
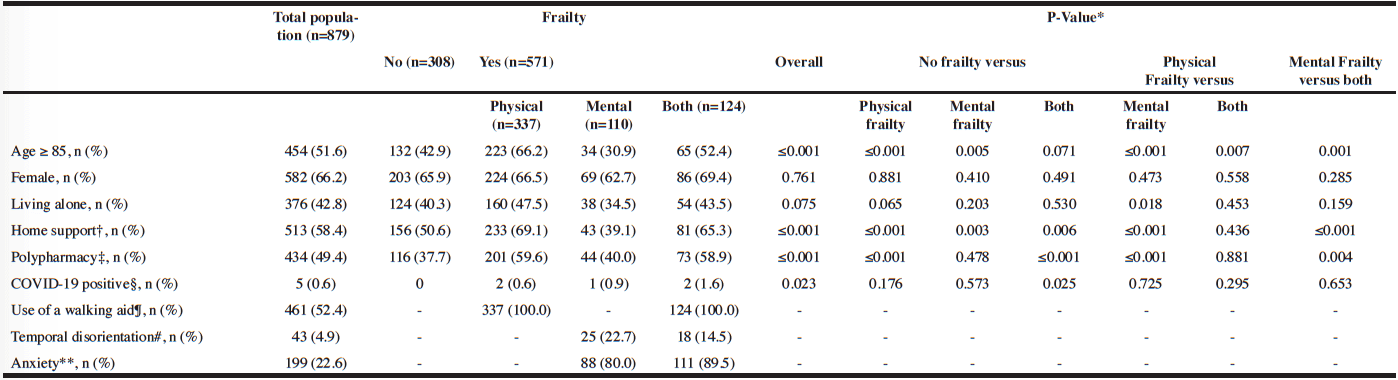
Table 1
Characteristics of participants separated into four groups based on their frailty phenotype (n=879)
*: based on Chi-squared test; †: Formal (i.e., health and/or social professionals) or informal (i.e., family and/or friends); ‡: Number of different medications taken daily ≥5; §: Older adults with at least 3 COVID-19 symptoms among fever ≥ 38°C /100°F, cough, shortness of breath and other symptoms; ¶: cane and rolling walker; #: Inability to give the month and/or year; **: Highest tertile of the verbal analogue anxiety scale score ranging from 0 (no anxiety) to 10 (severe anxiety).
These findings illustrate the high prevalence of frailty, especially of the physical phenotype, among homebound older community dwellers in Montreal. This result provides insight into the importance of prioritising preventive interventions that target insufficient physical activity in times of social distancing. Indeed, it is well known that older community dwellers with physical frailty are at increased risk for motor deconditioning and related adverse outcomes, which include muscle mass decline and increasingly unstable gait and balance, ultimately increasing the risk of falls and fractures (1). In this population, patient-centred care should include offering physical activity programs that take into account physical distancing measures (10). As suggested by Aubertin-Leheurdre & Rolland, innovative gerontechnology solutions such as exergames or web-based exercise programs may address the risk being homebound poses to older community dwellers (1).
Conflict of interest: The authors CPL, LCB, VI and OB report no disclosures relevant to the manuscript.
References
1. Aubertin-Leheurdre, Rolland Y. The importance of physical activity to care for frail older adults during the COVID-19 pandemic. J Am Med Dir Assoc. 2020 [Epub ahead of print].
2. Cudjoe TKM, Kotwal AA. «Social distancing» amidst a crisis in social isolation and loneliness. J Am Geriatr Soc. 2020 [Epub ahead of print]
3. WHO https://www.who.int/news-room/fact-sheets/detail/physical-activity (May 13, 2020 date last accessed)
4. Buttar HS, Li T, Ravi N. Prevention of cardiovascular diseases: Role of exercise, dietary interventions, obesity and smoking cessation. Exp Clin Cardiol. 2005;10:229-249.
5. Hubbard RE, Maier AB, Hilmer SN, Naganathan V, Etherton-Beer C, Rockwood K. Frailty in the Face of COVID-19. Age Ageing. 2020 [Epub ahead of print]
6. Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56:M146-156.
7. Kelaiditi E, Cesari M, Canevelli M, van Kan GA, Ousset PJ, Gillette-Guyonnet S, et al. Cognitive frailty: rational and definition from an (I.A.N.A./I.A.G.G.) international consensus group. J Nutr Health Aging. 2013;17:726-734.
8. Coronavirus Disease 2019 (COVID-19). Daily Epidemiology Update (Updated May 15, 2020, 2:00 PM ET). https://www.canada.ca/en/public-health/services/diseases/2019-novel-coronavirus-infection.html?utm_campaign=gc-hc-sc-coronavirus2021-ao-2021-0005-9834796012&utm_medium=search&utm_source=google_grant-ads-107802327544&utm_content=text-en-434601690158&utm_term=%2Bcoronavirus#a1
9. Beauchet O, Chabot J, Fung S, Launay CP. Update of the 6-Item Brief Geriatric Assessment Screening Tool of Older Inpatients at Risk for Long Length of Hospital Stay: Results From a Prospective and Observational Cohort Study. J Am Med Dir Assoc. 2018;19:720-721.
10. Bonadias Gadelha A, Lima RM. Letter to the Editor: COVID-19 Quarantine in Older People: The Need to Think about Sarcopenia-Related Phenotypes. J Frailty Aging. 2020;9(4):244-245.
