B. Everaars1,2, K. Jerković – Ćosić2, N. Bleijenberg3,4, N. J. de Wit4, G.J.M.G. van der Heijden1
1. Department of Social Dentistry, Academic Center for Dentistry Amsterdam (ACTA), University of Amsterdam and VU University, Amsterdam, The Netherlands; 2. University of Applied Sciences Utrecht, Research Group Innovations in Preventive Care; Utrecht, The Netherlands; 3. University of Applied Sciences Utrecht, Institute of Nursing Studies, Research Group Chronic Diseases; Utrecht, The Netherlands; 4. Utrecht University, University Medical Center Utrecht, Julius Center for Health Sciences and Primary Care, Utrecht, The Netherlands.
Corresponding author: B. Everaars, University of Applied Sciences Utrecht, Research Group Innovations in Preventive Care, Heidelberglaan 7, 3512 CS, Utrecht, The Netherlands, Email: babette.everaars@hu.nl, Telephone: 0614317567
J Frailty Aging 2021;10(1)56-62
Published online October 12, 2020, http://dx.doi.org/10.14283/jfa.2020.55
Abstract
Background: In frail older people with natural teeth factors like polypharmacy, reduced salivary flow, a decrease of oral self-care, general healthcare issues, and a decrease in dental care utilization contribute to an increased risk for oral complications. On the other hand, oral morbidity may have a negative impact on frailty. Objective: This study explored associations between oral health and two frailty measures in community-dwelling older people. Design: A cross-sectional study. Setting: The study was carried out in a Primary Healthcare Center (PHC) in The Netherlands. Participants: Of the 5,816 persons registered in the PHC, 1,814 persons were eligible for participation at the start of the study. Measurements: Two frailty measures were used: 1. Being at risk for frailty, using Electronical Medical Record (EMR) data, and: 2. Survey-based frailty using ‘The Groningen Frailty Indicator’ (GFI). For oral health measures, dental-record data (dental care utilization, dental status, and oral health information) and self-reported oral problems were recorded. Univariate regression analyses were applied to determine the association between oral health and frailty, followed by age- and sex-adjusted multivariate logistic regressions. Results: In total 1,202 community-dwelling older people were included in the study, 45% were male and the mean age was 73 years (SD=8). Of all participants, 53% was at risk for frailty (638/1,202), and 19% was frail based on the GFI (222/1,202). A dental emergency visit (Odds Ratio (OR)= 2.0, 95% Confidence Interval (CI)=1.33;3.02 and OR=1.58, 95% CI=1.00;2.49), experiencing oral problems (OR=2.07, 95% CI=1.52;2.81 and OR=2.87, 95% CI= 2.07;3.99), and making dietary adaptations (OR=2.66, 95% CI=1.31;5.41 and OR=5.49, 95% CI= 3.01;10.01) were associated with being at risk for frailty and survey-based frailty respectively. Conclusions: A dental emergency visit and self-reported oral health problems are associated with frailty irrespective of the approach to its measurement. Healthcare professionals should be aware of the associations of oral health and frailty in daily practice.
Key words: Dental care for aged, frailty, oral health, primary health care.
Introduction
After decades of a decline in the prevalence of edentulous people of older age, this decline seems to have stalled (1, 2). In older people with natural teeth factors like polypharmacy, reduced salivary flow, a decrease of oral self-care, general healthcare issues, and a decrease in dental care utilization contribute to an increased risk for oral complications (3-5). These clinical and lifestyle factors together with demographic, social and biological factors are present in the onset of frailty (6). Frailty is a progressive condition mostly at a higher age, that is associated with adverse health outcomes including functional decline, long-term care and a higher risk of mortality (7, 8).
Few studies investigated the association between oral health and frailty (or a domain thereof). The most recent review of Hakeem et al. (2019) including only longitudinal studies, showed associations between number of teeth and masticatory function on the one hand, and frailty on the other hand (9). Another review including only cross-sectional studies reported associations between, on the one hand, the need for a dental prosthesis, self-reported oral health, dental service use, oral health-related quality of life, and on the other hand frailty (its physical component). But associations for frailty with number of teeth, masticatory function and periodontitis were not found (10).
The above-mentioned reviews used the unidimensional Fried frailty phenotype to determine frailty. However, studies exploring the association between oral health and multi-dimensional frailty measures are lacking (9, 11). Therefore, the aim of this study was to explore the association between oral health and frailty using two frailty measures: (1) based on Electronical Medical Record (EMR) data and (2) frailty based on survey data in community-dwelling older people.
Methods
For reporting this cross-sectional study we applied the relevant items of Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement (12).
Design and setting
This cross-sectional study was carried out in a Primary Healthcare Center (PHC) in The Netherlands. The multidisciplinary PHC team consists of general practitioners (GP), practice nurses, health care assistants, a pharmacist, dentists, and dental hygienists.
Participants and study sample
Of the 5,816 persons registered in the PHC, 1,842 were 60 years of age or older at the start of the study. The GP or practice nurse considered 28 persons unable to participate because of cognitive or physical constraints, whereby 1,814 persons were considered eligible for participation in the study.
Data collection procedures
All 1,814 persons were invited to participate in the study in April 2016. They received an information letter from the GP and were asked for informed consent to extract dental record data and to match these data with their routine healthcare data. We asked if and in which dental clinic the participants were registered, in order to retrieve dental record data. In addition, participants were asked to complete a questionnaire on self-reported frailty. If individuals agreed to participate in the study but information on their dental clinic was missing, this was obtained by phone. After receiving informed consent, dental record data from 1.5 years prior to the consent was collected. This period of 1.5 years was arbitrary chosen because it is considered as a dental consultation gap: around 75% of the Dutch citizens visit the dentist every year (13).
For participants registered in the dental clinic within the same primary healthcare center (81%), the research assistant manually collected the dental record data. For participants registered in other dental clinics in the Netherlands (19%), data were obtained from the dentist via a structured data extraction form.
Frailty indicators
Frailty identification
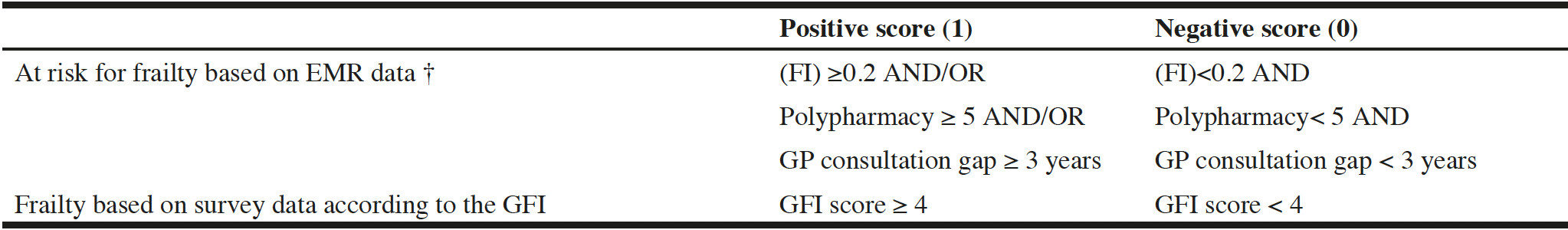
Frailty was assessed by two validated measures. First, we used the Utrecht Periodic Risk Identification and Monitoring system (U-PRIM). The U-PRIM was designed to classify older people at risk for frailty. The U-PRIM extracts data from the EMR on multi-morbidity to calculate the Frailty Index (FI) (14), polypharmacy and a possible GP consultation gap. The FI is calculated out of the proportion of 50 potential health deficits defined by the presence of one or more International Classification of Primary Care (ICPC) and diagnosis and prescription (Anatomic Therapeutic Chemical (ATC)) codes (ranging from zero (fit) to one (frail)) (14-16). A cut-off of 0.2 distinguished between a positive or negative FI score (see Table 1). Polypharmacy was defined as the chronic use of five or more different kinds of medications according to the ATC coding. A GP consultation gap was denoted as present when someone did not visit the GP for 3 or more years (with the exception of the annual influenza vaccination). For the purpose of analyses, frailty based on the U-PRIM variables was dichotomized: older people at risk for frailty vs. older people not at risk for frailty. People were considered at risk for frailty if they scored positive on either the FI, polypharmacy or GP consultation gap. The only possibility to be classified as not at risk for frailty was to score negative on all three variables. For a detailed coding scheme, see Table 1.
Second, a self-administered survey on self-reported frailty was filled out: i.e. frailty based on survey data. For this, the Groningen Frailty Indicator (GFI) was used. The GFI is a Dutch validated questionnaire consisting of 15 questions regarding the physical, cognitive, social and psychological domains (17). Each question was rated as 0 (negative) or 1 (positive) with a total score ranging from 0 to 15. Results were dichotomized in frail based on survey data (a total GFI score of 4 or higher) vs. not frail based on survey data (a GFI score lower than 4) (see Table 1) (17).
† Someone was not potentially frail if scoring negative on all three variables (FI, Polypharmacy, and GP consultation gap).
Oral health indicators
Dental record data and self-reported oral problems were collected. The information on self-reported oral problems was collected together with the GFI questions and concerned two questions: 1. Do you experience pain, a dry mouth or other discomforts in your mouth? 2. Did you change your food choices because of this discomfort in your mouth? Response categories ‘’sometimes’’ and ‘’yes’’ were dichotomized into positive (1), and answers ‘’no’’ were scored negative (0).
Participants who stated to not visit/being registered in a dental clinic the past 1.5 years, were categorized as having a dental consultation gap. If participants had no dental consultation gap, additional dental information within the timeframe of 1.5 years was extracted: the dental status (natural teeth (reference), partial prosthesis, full prosthesis), dental treatments: extraction (yes=1/no=0), caries treatment (yes=1/no=0), emergency treatment (yes=1/no=0) and periodontal problems were extracted. Periodontal status was categorized according to the Dutch Periodontal Index (DPSI) (18). Category A+B indicated no/minor periodontal disease (0) whereas category C referred to periodontal disease (1). Dental visit was recoded into a dental consultation gap: visited the dentist within the past 1.5 years (0) and did not visit the dentist within the past 1.5 years (1).
Statistical analysis
Descriptive data were calculated separately for participants being at risk for frailty or not, and for those who were frail versus non-frail according to the GFI questionnaire. The following descriptive statistics were calculated: mean and standard deviation (SD) (continuous and normally distributed data), median and interquartile range (IQR) (non-normally distributed data), and percentages (nominal scale) were reported. To compare the groups, t-tests, chi-square tests and a Mann-Whitney U test were performed (see footnote in Table 2).
To explore the associations between oral health and both frailty measures, univariate logistic regression analyses were performed on all oral health variables and the covariates. Subsequently, a multivariate logistic regression analysis was performed adjusted for age and sex. For all statistical analyses, a p-value of ≤0.05 was considered significant. Analyses were performed with SPSS version 24.0.
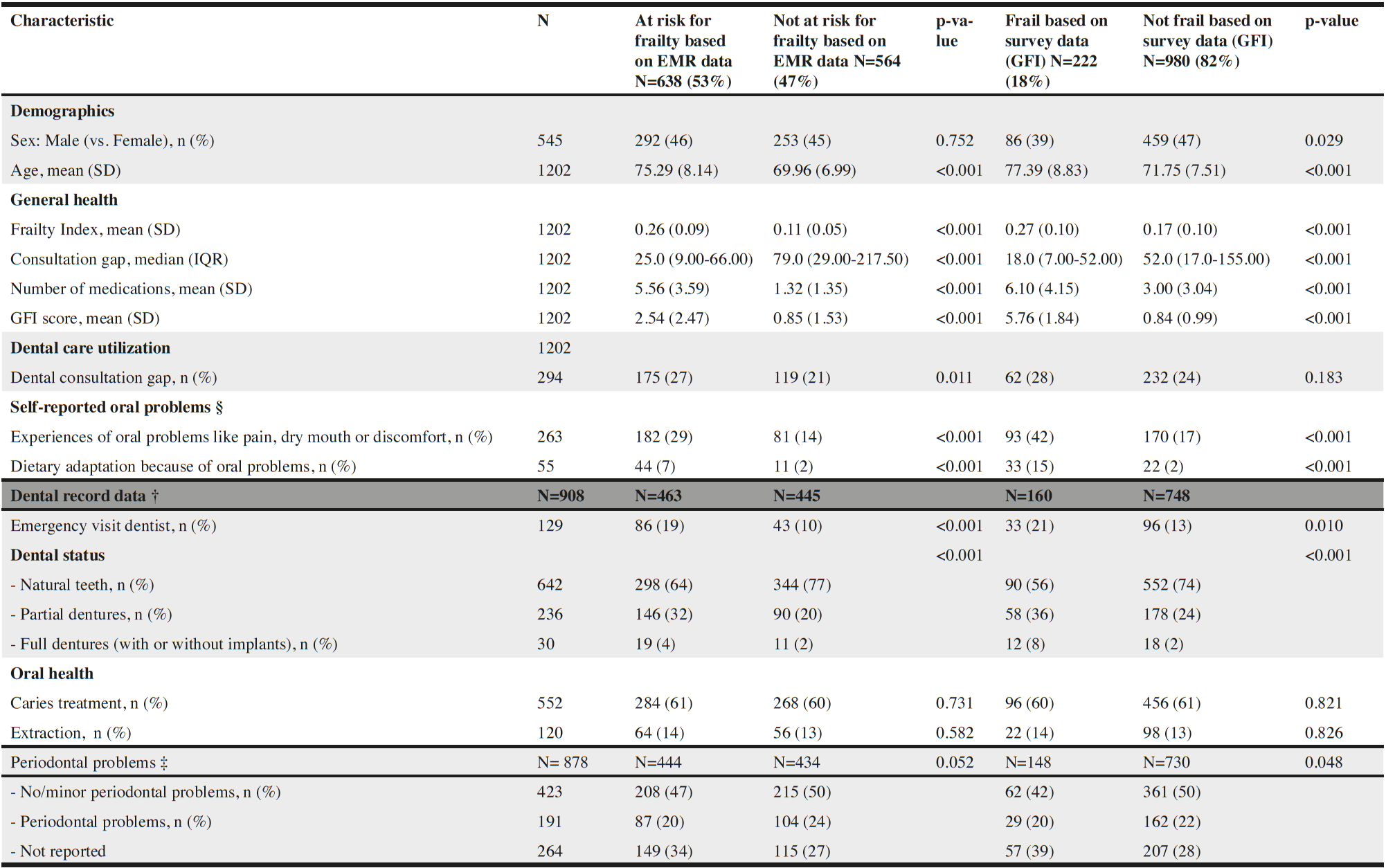
Table 2
Descriptive baseline data on general health and oral health distinguished for people at risk for frailty (based on EMR data) and frailly based on survey data (GFI)
Note: SD=standard deviation; IQR=inter quartile range; Statistical tests: for the variables: Sex, Dental consultation gap, Self-reported oral problems and all dental record data (nominal scale) a chi-square test was performed; For: Age, Frailty Index, Number of medications, and GFI score (ratio scale) a t-test was performed. For the variable: consultation gap (compare medians) the Mann-Whitney U test was performed; §. Self-reported oral problems had 8 missing cases for experiences of oral problems and 9 missing cases for food adaptation. Analysis have been performed on full data: respectively N=1194 and N=1193. †. From 908 participants we retrieved dental record data. In case of a consultation gap or if people were not registered in a dental practice, no dental record was available from the past 1.5 years. The proportion of dental record data and statistical test are calculated based on the total N=908. ‡. Periodontal information was not available for people with full prosthesis (on implants) and were excluded for analysis. The proportion of periodontal information and statistical tests are calculated based on the total N=878.
Missing data
Participants with five or more missing items on their GFI questionnaire, were excluded for analysis. For dental record data, full data analysis was performed: participants without a registration in a dental clinic or with a dental consultation gap no additional dental record data were available and were excluded for analysis.
Twelve participants had missing data on either one or two self-perceived oral health questions. For these participants, full data-availability analysis was performed.
Regarding periodontal health, the DPSI score was not documented by dentists in many cases. A sensitivity analysis showed that the inclusion of these missing variables as an individual risk factor provided us with the most informative results.
Ethics
The Medical ethics Review board of UMC Utrecht decided to provide a waiver for the study from full assessment according to the Medical Research Involving Human Subjects Act (WMO) (reference: WAG/mb/16/013553). During the study, the study team adhered to the General Data Protection Regulation (GDPR).
Results
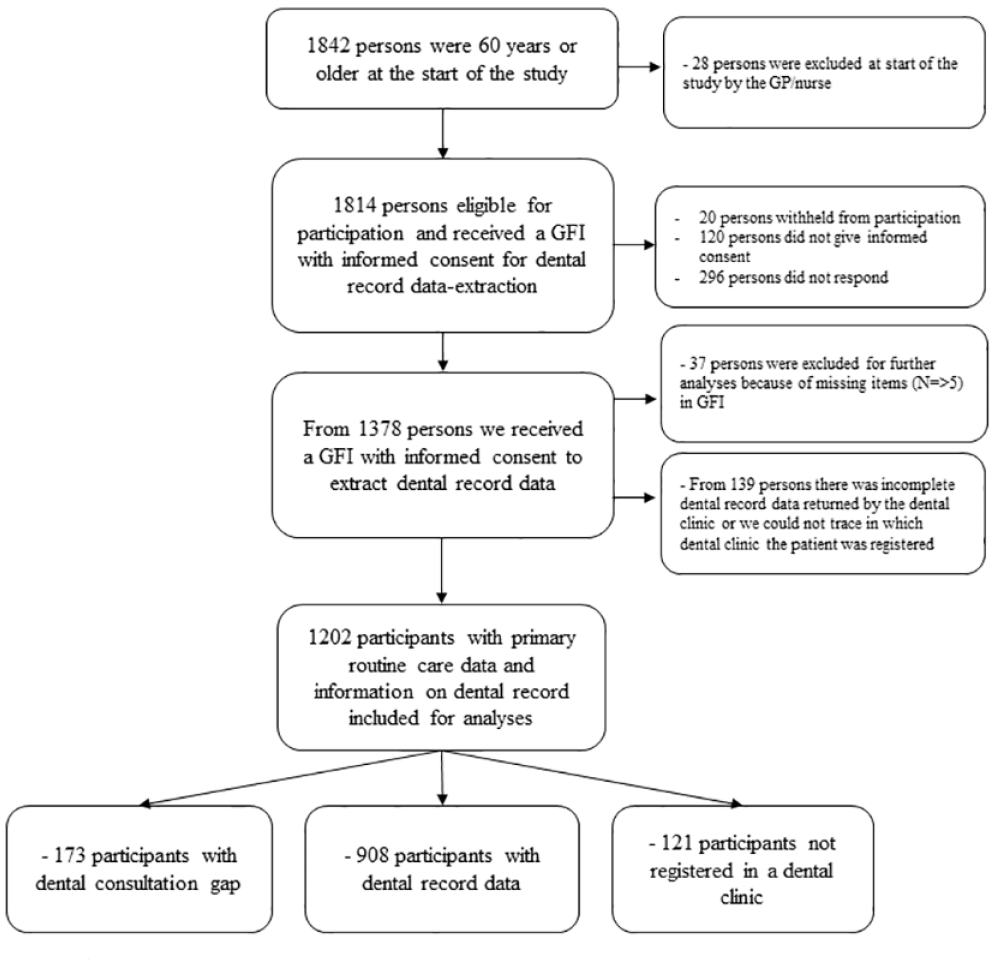
Of the 1,814 persons eligible for study participation, 1,378 provided consent. In total, 1,202 were included in the study. A flowchart for in- and exclusion is shown in Figure 1.
Demographics and General health factors
Of the 1,202 participants, 545 (45%) were male. The mean age of participants was 73 years (SD=8). Based on EMR data 638 (53%) of the older people were at risk for frailty: 554 (46%) scored positive on the FI, 397 (33%) scored positive on polypharmacy and 22 (2%) scored positive on a GP consultation gap. Based on survey data, 222 (18%) were considered frail. People at risk for frailty according to EMR data were generally older, had a higher FI score, used more medications, had a higher GFI mean score and had a shorter GP consultation gap compared to participants not at risk (Table 2). Frail older people based on survey data according to the GFI showed comparable characteristics (Table 2).
Oral health
Out of 1,202 participants, we retrieved from 908 (76%) participants dental record data (Figure 1). From 294 (24%) participants we could not retrieve dental record data because 121 (41%) of them were not registered in a dental clinic and 173 (59%) of them did not visit their dentist the past 1.5 years (see Figure 1). In 264 (29%) participants, no DPSI score had been registered by the dental professional in the timeframe of 1.5 years (missing data).
We found significant differences in oral health between participants at risk for frailty based on EMR data and participants not at risk. For those at risk for frailty compared to those not at risk, larger proportions had a dental consultation gap (27% vs. 21%), experienced oral problems (29% vs. 14%), made dietary adaptations because of oral problems (7% vs. 2%), had a dental emergency visit (19% vs. 10%) and had partial- (32% vs. 20%) or full prosthesis (4% vs. 2%) (see Table 2).
Frail participants based on survey data according to the GFI showed also significant differences in oral health compared to the non-frail participants. For frail participants compared to non-frail participants, larger proportions experienced oral problems (42% vs. 17%), made dietary adaptations because of oral problems (15% vs. 2%), had a dental emergency visit (21% vs.13%), had a partial (36% vs. 24%) or full prosthesis (8% vs. 2%), and missing periodontal information (39% vs. 28%) (see Table 2). No significant differences were found for caries treatment and tooth extraction between the groups, with respectively risk of frailty based on EMR data and survey based frailty (according to the GFI) (see Table 2).
Associations between oral health and frailty
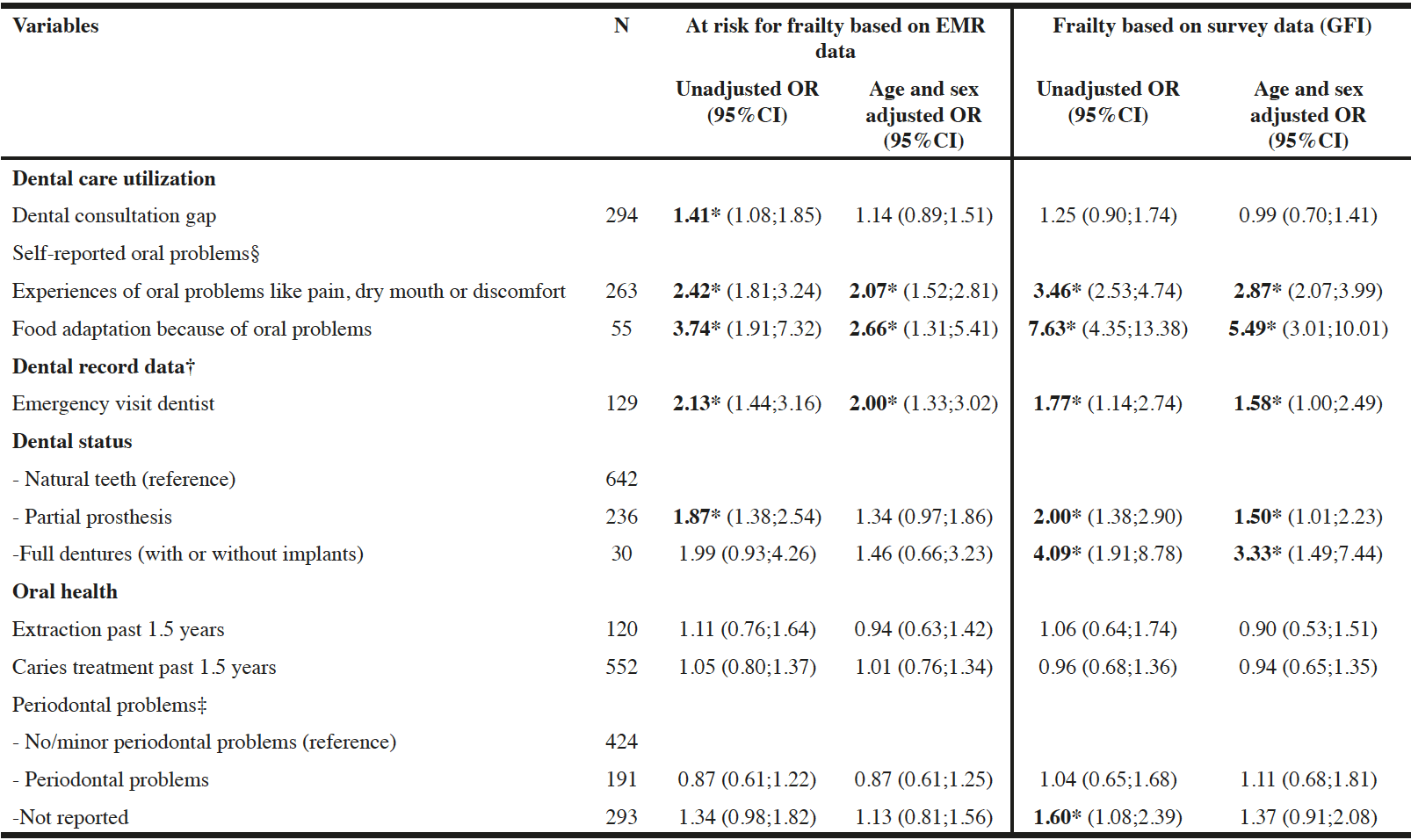
Associations (adjusted for age and sex) between frailty based on EMR data and oral health were found. Participants at risk for frailty, compared to participants not at risk had a higher chance on experiencing oral discomfort (OR=2.07, 1.52;2.81), making dietary adaptations (OR=2.66, 1.31;5.41) and consulting an emergency dental visit (OR=2.00, 1.33;3.02) (see Table 3).
Similar associations were found for frail participants based on survey data according to the GFI (including adjustment for age and sex) compared to non-frail participants: they had a higher chance of experiencing oral discomfort, making dietary adaptations and an emergency dental visit. In addition, they had a higher chance of having a partial or full prosthesis. The strongest associations were found between frailty based on survey data according to the GFI and making dietary adaptations and wearing a full prosthesis (see Table 3). Frail participants were 5.5 times more likely (OR 5.49, 95% CI 3.01; 10.01) of making dietary adaptations because of oral problems and 3.3 times more likely wearing full prosthesis (OR 3.33, CI 1.49;7.44).
§. self-reported oral problems had 8 missing cases for experiences of oral problems and 9 missing cases for food adaptation. Analysis have been performed on full data: respectively N=1194 and N=1193; †. Analysis were performed on 908 participants. In case of a consultation gap or if people were not registered in a dental practice, no dental record was available from the past 1.5 years. The proportion of dental record data and statistical test are calculated based on the total N=908; ‡. Periodontal information was not available for people with full prosthesis (on implants) and were excluded for analysis. The analysis were performed on N=878 participants; * Significant association P≤0.05
Discussion
This study identifies the associations between oral health and two frailty measures in community-dwelling older people. A dental consultation gap, an emergency dental visit, wearing a (partial) prosthesis and self-reported oral health problems are associated with one or both frailty measures. The strongest associations were found between frailty based on survey data according to the GFI on the one hand and making dietary adaptations and wearing a full prosthesis on the other hand.
Our findings are supported by studies showing similar patterns regarding oral health and frailty measures. Although the association between risk of frailty and having less natural teeth has been reported for most studies included in the review by Torres et al. (2015) (10) and three cross-sectional studies (18-20), the definitions and measures that have been used among these studies on oral health and frailty differ to a large extent. Therefore it remains difficult to compare the results of these studies. This accounts also for the associations between frailty and periodontal information. In contrast to other studies, we extracted information on periodontal status from dental records and did not perform a clinical periodontal assessment (10).
Moreover, it has been reported that frail people in the Netherlands tend to seek less dental care because of giving higher priority to other health care issues than oral health problems (3, 21).
Strengths and limitations
In this study, we strived to use data that is objective and easy to be extracted in daily practice. However, some limitations need to be considered to appreciate our findings. First, the dental record data were extracted manually from the dental records. While in some instances availability of dental record data was limited and registration was poor, data collection was successful in the majority of persons consenting for participation. Second, by collecting self-reported oral health problems we obtained information that is not routinely reported by dentists, like xerostomia (5). Last, this research was performed in an area with a high density of people with high socio-economic status (SES), with a mean score of 0.89 compared to the rest of the Netherlands (mean 0.17) (23). Since a low socio-economic status has shown to negatively impact oral health and frailty, we need to take into account an underestimation of the prevalence of oral health problems and frailty in our results compared to the general population (24).
Implications for practice, policy, and research
Based on the findings of our study as well as other recent studies (10, 25, 26) we suggest incorporating dental record data in the frailty screening of older community-dwelling people.
Besides the self-reported oral health problems, including dental record data might be useful in predicting frailty, as this is an easy and low-cost way to gather patients’ oral health information. However, to do so, it is necessary for dental clinic to systematically record the patients’ dental care utilization, oral health status, and problems. Standardized documentation of this information is needed, to enable healthcare workers to use multi-disciplinary information in frailty detection and proactive care programs. The same accounts for future research.
The World Dental Federation (FDI) has published a uniform definition of oral health and currently is working on a standardized set of oral health measures (27), which could be adopted in the context of dental care for frail older people. However, to date, the predictive prognostic value of oral health in the early frailty risk detection of community-dwelling older persons has not been shown and the development of such a prognostic prediction model is warranted.
In conclusion, an emergency visit at the dentist and self-reported oral health problems are associated with frailty irrespective of the approach to its measurement. To improve understanding of the relationship between oral health and frailty in community-dwelling older persons, follow-up research with large study populations is needed. The data-collection of these studies should stay close to what healthcare professionals routinely document and it is recommended to include dental record data and self-reported oral health problems in the prognostic prediction models derived thereof.
Acknowledgments: We gratefully acknowledge the professionals from the Primary Healthcare Center for collaboration during the research project, the student-assistants who participated in the data collection procedures, and all dental clinics who participated in extracting dental record data on their patients.
Funding: This study was performed without funding.
Conflict of interest: Ms. Babette Everaars has nothing to disclose. Dr. K. Jerković – Ćosić has nothing to disclose. Dr. N. Bleijenberg has nothing to disclose. Dr. N.J. de Wit has nothing to disclose. Dr. G.J.M.G. van der Heijden has nothing to disclose.
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. Slade GD, Akinkugbe AA, Sanders AE. Projections of U.S. Edentulism Prevalence Following 5 Decades of Decline. Journal of Dental Research. 2014 Oct;93(10):959-65.
2. Wu B, Liang J, Plassman BL, Remle C, Luo X. Edentulism trends among middle-aged and older adults in the United States: comparison of five racial/ethnic groups. Community Dent Oral Epidemiol. 2012 Apr;40(2):145-53.
3. Niesten D, Witter DJ, Bronkhorst EM, Creugers NHJ. Oral health care behavior and frailty-related factors in a care-dependent older population. J Dent. 2017 Jun;61:39-47.
4. Ohi T, Sai M, Kikuchi M, Hattori Y, Tsuboi A, Hozawa A, et al. Determinants of the utilization of dental services in a community-dwelling elderly Japanese population. Tohoku J Exp Med. 2009 Jul;218(3):241-9.
5. Ramsay SE, Papachristou E, Watt RG, Tsakos G, Lennon LT, Papacosta AO, et al. Influence of Poor Oral Health on Physical Frailty: A Population-Based Cohort Study of Older British Men. J Am Geriatr Soc. 2018 Mar;66(3):473-9.
6. Hoogendijk EO, Afilalo J, Ensrud KE, Kowal P, Onder G, Fried LP. Frailty: implications for clinical practice and public health. Lancet. 2019 Oct 12;394(10206):1365-75.
7. Slaets JPJ. Vulnerability in the elderly: frailty. Med Clin North Am. 2006 Jul;90(4):593-601.
8. Rockwood K. Frailty and its definition: a worthy challenge. J Am Geriatr Soc. 2005 Jun;53(6):1069-70.
9. Hakeem FF, Bernabe E, Sabbah W. Association between oral health and frailty: A systematic review of longitudinal studies. Gerodontology. 2019 Sep;36(3):205-15.
10. Torres LH, Tellez M, Hilgert JB, Hugo FN, de Sousa MD, Ismail AI. Frailty, Frailty Components, and Oral Health: A Systematic Review. J Am Geriatr Soc. 2015 Dec;63(12):2555-62.
11. Roppolo M, Mulasso A, Gobbens RJ, Mosso CO, Rabaglietti E. A comparison between uni- and multidimensional frailty measures: prevalence, functional status, and relationships with disability. Clin Interv Aging. 2015 Oct 22;10:1669-78.
12. von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. PLoS Med. 2007 Oct 16;4(10).
13. Ongeveer drie kwart bezoekt jaarlijks huisarts en tandarts. 2013. Available from: https://www.cbs.nl/nl-nl/nieuws/2013/27/ongeveer-drie-kwart-bezoekt-jaarlijks-huisarts-en-tandarts. Accessed 7 May 2019
14. Drubbel I, Bleijenberg N, Kranenburg G, Eijkemans RJ, Schuurmans MJ, de Wit NJ, et al. Identifying frailty: do the Frailty Index and Groningen Frailty Indicator cover different clinical perspectives? a cross-sectional study. BMC Fam Pract. 2013 May 21;14:64-.
15. Bleijenberg N, Drubbel I, Schuurmans MJ, Dam HT, Zuithoff NP, Numans ME, et al. Effectiveness of a Proactive Primary Care Program on Preserving Daily Functioning of Older People: A Cluster Randomized Controlled Trial. J Am Geriatr Soc. 2016 Sep;64(9):1779-88.
16. Rockwood K, Song X, Macknight C, Bergman H, Hogan DB, McDowell I, Mitnitski A. A global clinical measure of fitness and frailty in elderly people. Can Med Assoc J. 2005:9-13.
17. Schuurmans H, Steverink N, Lindenberg S, Frieswijk N, Slaets JP. Old or frail: what tells us more? J Gerontol A Biol Sci Med Sci. 2004 Sep;59(9):962.
18. Van der Velden U. The Dutch periodontal screening index validation and its application in The Netherlands. J Clin Periodontol. 2009 Dec;36(12):1018-24.
19. Watanabe Y, Hirano H, Arai H, Morishita S, Ohara Y, Edahiro A, et al. Relationship Between Frailty and Oral Function in Community-Dwelling Elderly Adults. J Am Geriatr Soc. 2017 Jan;65(1):66-76.
20. Hasegawa Y, Sakuramoto A, Sugita H, Hasegawa K, Horii N, Sawada T, et al. Relationship between oral environment and frailty among older adults dwelling in a rural Japanese community: a cross-sectional observational study. BMC Oral Health. 2019 Jan 22;19(1):23-8.
21. de Andrade FB, Lebrao ML, Santos JL, Duarte YA. Relationship between oral health and frailty in community-dwelling elderly individuals in Brazil. J Am Geriatr Soc. 2013 May;61(5):809-14.
22. Niesten D, van Mourik K, van der Sanden W. The impact of frailty on oral care behavior of older people: a qualitative study. BMC Oral Health. 2013 Nov 1;13:61-.
23. Ontwikkeling Sociaal Economische Status (SES) Utrechtse Heuvelrug, GGD Utrecht en Nederland 1998-2010.1998. https://www.rivm.nl/media/profielen/profile_1581_Utrechtse_Heuvelrug_omgeving.html. Accessed 22 Feb 2019
24. Donaldson AN, Everitt B, Newton T, Steele J, Sherriff M, Bower E. The Effects of Social Class and Dental Attendance on Oral Health. J Dent Res. 2008;87(1):60-4.
25. Tanaka T, Takahashi K, Hirano H, Kikutani T, Watanabe Y, Ohara Y, et al. Oral Frailty as a Risk Factor for Physical Frailty and Mortality in Community-Dwelling Elderly. The journals of gerontology. Series A, Biological sciences and medical sciences. 2018 Nov 10,;73(12):1661-7.
26. Castrejon-Perez RC, Jimenez-Corona A, Bernabe E, Villa-Romero AR, Arrive E, Dartigues JF, et al. Oral Disease and 3-Year Incidence of Frailty in Mexican Older Adults. J Gerontol A Biol Sci Med Sci. 2017 Jul 1;72(7):951-7.
27. FDI and ICHOM present Standard Set of Adult Oral Health Measures. 2018. https://www.fdiworlddental.org/news/20180908/fdi-and-ichom-present-standard-set-of-adult-oral-health-measures. Accessed 2 April 2019